Epidemiology: Vascular biology, endothelial and vascular smooth muscle as well as cardiac dysfunction play a primary role in hypertension, cardio-vascular disease and target organ damage. Nutrient-gene interactions and epigenetics are predominant factors in promoting positive and negative effects in cardiovascular health and hypertension. In a series of research studies correlated to cardiovascular disease and hypertension, Dr. Mark C. Houston, MD, discussed the role that vascular biology and nutraceuticals play in relation to treatment of hypertension and cardiovascular disease.
Table of Contents
What is the cause of cardiovascular disease and hypertension?
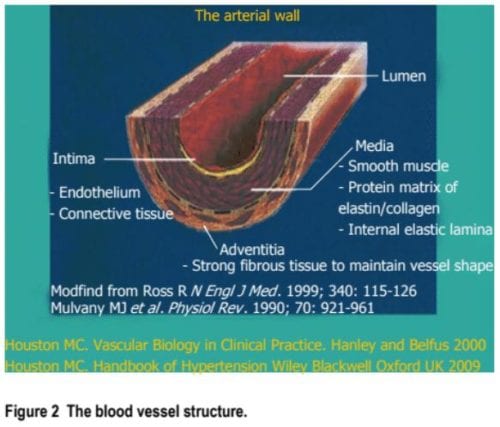
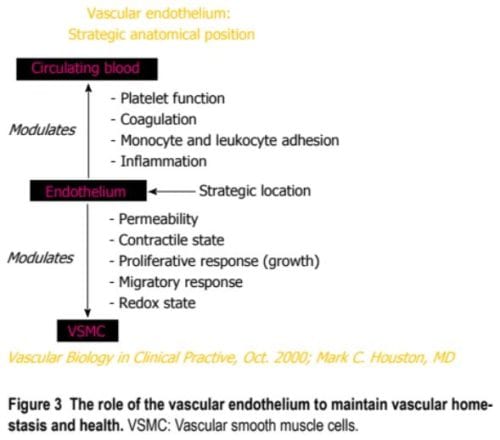
Vascular disease can appropriately be described as the balance between vascular injury and vascular repair (Figure 1). The endothelium is strategically found to be closely associated to the bloodstream as well as the vascular smooth muscle and it is also in charge of discharging a variety of substances in order to preserve vascular homeostasis and health (Figures 2 and 3). Numerous irritations which can provoke damage or harm to the endothelium, can lead to endothelial dysfunction, or ED, and can cause hypertension and other cardiovascular diseases.
Hypertension might be a hemodynamic indication of a damaged or injuried endothelium and vascular smooth muscle which could be connected to definite inflammation responses, oxidative stress and immune dysfunction of the arteries leading to ED, vascular and cardiac smooth muscle disorder, loss of arterial elasticity together with reduced arterial compliance and increased systemic vascular resistance. Hypertension is a significant outcome of the interaction between environmental factors and genetics. Macronutrients and micronutrients are crucial in the regulation of blood pressure, or BP, following target organ damage, or TOD. Nutrient-gene interactions, subsequent gene expression, epigenetics, oxidative stress, inflammation and autoimmune vascular dysfunction have positive or negative influences on vascular biology in humans. Endothelial activation with endothelial dysfunction and vascular smooth muscle breakdown, or VSMD, can ultimately trigger and continue to stimulate the development and growth of hypertension.
Macronutrient and micronutrient deficiencies are extremely common in the general population and may be even more common in individuals with hypertension and cardiovascular disease associated with genetics, environmental factors and even prescription drug and medication usage. These deficiencies have an enormous impact on cardiovascular health issues, such as hypertension, myocardial infarction, or MI, stroke and renal disease. The diagnosis and treatment of those deficiencies will reduce BP and improve ED, vascular biology and health, as well as cardiovascular function.
Epidemiology
Epidemiology, the branch of medicine that deals with the incidence, distribution, and possible control of diseases and other factors relating to health, emphasizes the role of diet and related nutritional intake when it comes to hypertension and cardiovascular disease. The transition from the Paleolithic diet to our modern diet has produced an outbreak of nutritionally-related diseases (Table 1). Hypertension, atherosclerosis, coronary heart disease, or CHD, MI, congestive heart failure, or CHF, cerebro-vascular accidents, or CVA, renal disease, type 2 diabetes mellitus, or T2DM, metabolic syndrome, or MS, and obesity are several examples of those diseases. Table 1 contrasts intake of nutrients included during the Paleolithic Era and modern time, involved in the regulation of blood pressure, or BP. An unnatural and unhealthy nutritional selection process has been established by evolution from a pre-agricultural, hunter-gatherer milieu into an agricultural, refrigeration society. In sum, diet has changed more than our genetics can adapt.
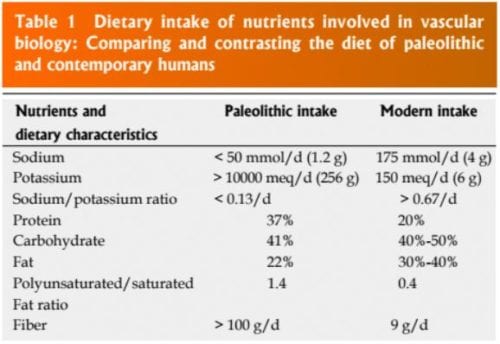
The human genetic makeup is approximately 99.9 percent that of our Paleolithic ancestors, however our nutritional, vitamin and mineral intakes have vastly changed. The macronutrient and micronutrient variations, oxidative stress from radical oxygen species, or ROS, and radical nitrogen species, or RNS, and inflammatory mediators, such as cell adhesion molecules, or CAMs, cytokines, signaling molecules and autoimmune vascular dysfunction of T cells and B cells, have contributed to the greatest prevalence of hypertension and other cardiovascular diseases through complex nutrient-gene interactions, epigenetic and nutrient-caveolae interactions and nutrient responses with pattern recognition receptors from the endothelium (Figure 4). A decrease in endothelin coupled with endothelial activation, increase in angiotensin II and nitric oxide bioavailability can cause coronary artery disease and vascular disease as well as hypertension. Poor nutrition, together with obesity and a sedentary lifestyle have led to an exponential increase in nutritionally-related ailments. In particular, the high Na+/K+ ratio of contemporary diets has contributed to hypertension, CVA, CHD, MI, CHF and renal disorder as have the relatively low intake of omega-3 PUFA, increase in omega-6 PUFA, saturated fat and trans fatty acids.
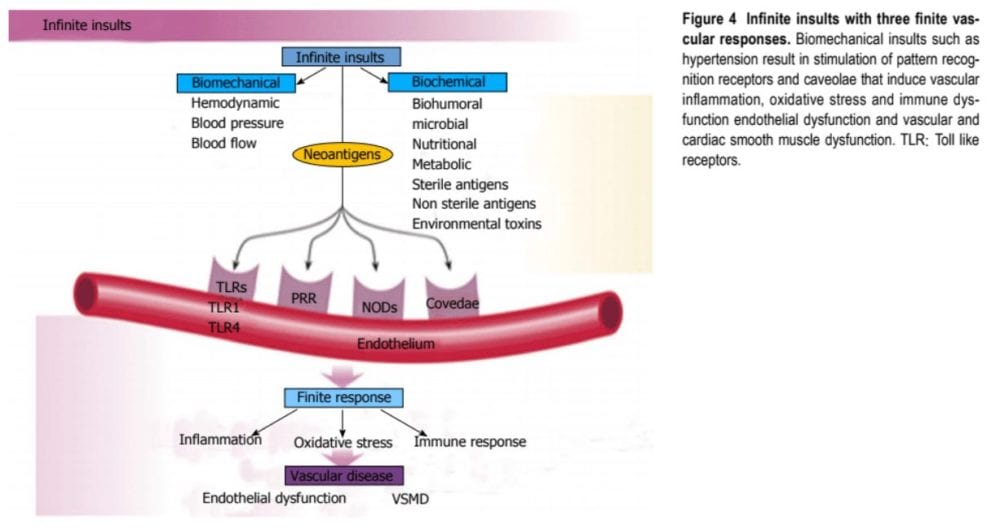
Pathophysiology
Vascular biology plays a major role in the initiation and perpetuation of hypertension. Oxidative stress (both ROS and RNS), inflammation and autoimmune vascular dysfunction (both T cells and B cells) are the primary pathophysiologic and functional mechanisms that cause cardiovascular disease (Figure 5). All three of them are closely interconnected and provide the absolute combination that leads to cardiovascular disease, or CVD, vascular smooth muscle and cardiac dysfunction, hypertension, vascular disease, atherosclerosis and endothelial dysfunction, or ED.
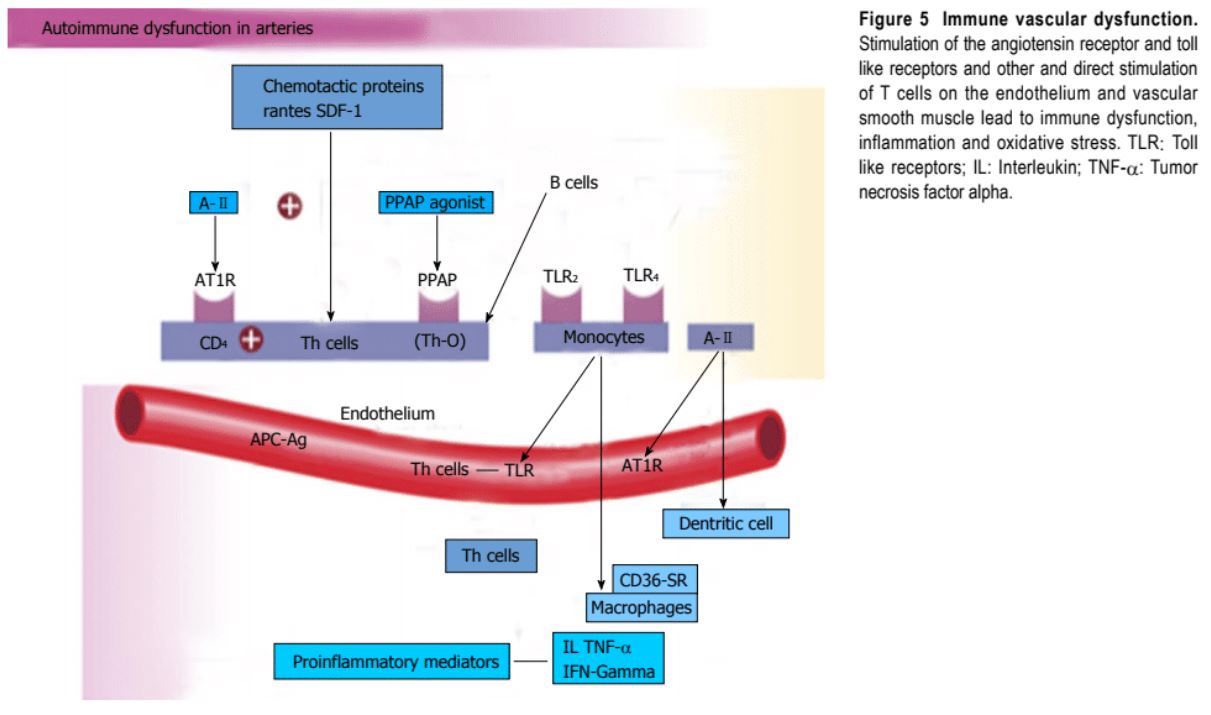
Hypertension is not a disease but is the proper and continuous, unregulated reaction with an exaggerated outcome of the infinite irritations to the blood vessel following environmental-genetic expression patterns and downstream disturbances in which the vascular system is the innocent bystander. This really becomes a maladaptive vascular response that was initially meant to provide vascular defense to the endothelial insults (Figure 6). Hypertension is a vasculopathy, characterized by ED, structural remodeling, vascular inflammation, improved stiffness, decreased distensibility and loss of elasticity. These insults are biomechanical (BP, heartbeat, blood circulation, oscillatory flow, turbu-lence, enhancement, pulse wave velocity and reflected waves) and biohumoral or biochemical which includes all the non-mechanical causes like metabolic, endocrine, nutritional, toxic, infectious and other etiologies.
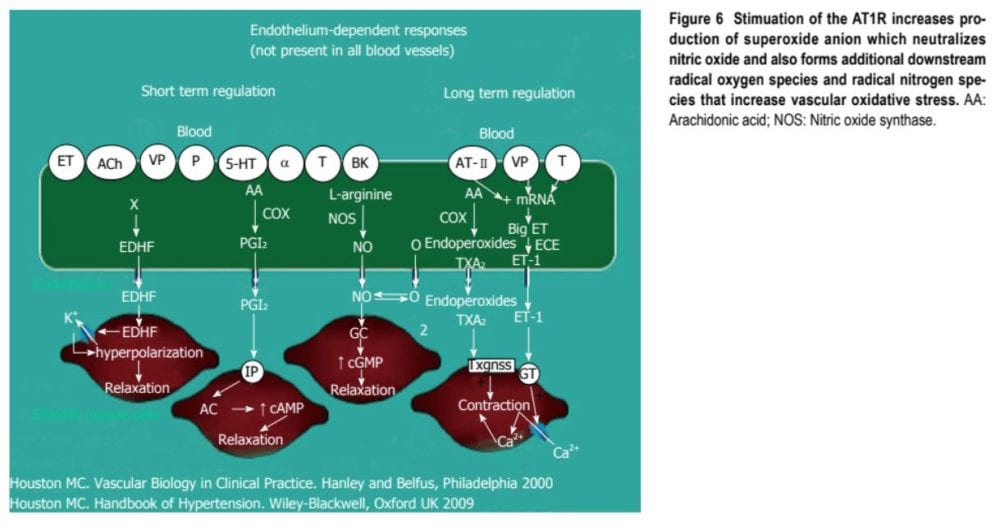
In addition to the connections for endocrine and nutritional causes of hypertension, infections and toxins can increase blood pressure as well. Various toxins, such as mercury, polychlorinated biphenyls, lead, cadmium, arsenic and iron, also increase BP and CVD. Numerous microbial organisms have also been implicated in hypertension and CHD. All of these irritations lead to the altered vascular structure and function that manifests clinically as hypertension. Patients with hypertension have abnormal microvasculature in the form of inward eutrophic remodeling of the tiny resistance arteries leading to impaired vasodilatory capacity, increased cardiovascular disease, increased media to lumen ratio, decreased maximal organ perfusion and decreased flow reserve, particularly in the heart with decreased coronary flow reserve. Significant functional structural microvascular impairment occurs even before the individual’s blood pressure begins to increase in normotensive offspring of the patients with hypertension, as evidenced by endothelial dysfunction, diminished vasodilation, forearm vascular resistance, diastolic dysfunction, increased left ventricular mass index, increased septal and posterior wall thickness and left untreated hypertrophy. Therefore, the processes underlying the circulatory issues are associated to a vascular phenotype of hypertension that may be determined by early life programming and imprinting which may be compounded by cerebral aging.
In conclusion, vascular biology, endothelial and vascular smooth muscle as well as cardiac dysfunction play a primary role in hypertension, cardio-vascular disease and target organ damage. Then, the epidemiology, or the incidence, distribution, and possible control of diseases and other factors relating to health, emphasizes the role of diet and related nutritional intake when it comes to hypertension and cardiovascular disease. And finally, oxidative stress, inflammation and autoimmune vascular dysfunction are the primary pathophysiologic and functional mechanisms that cause cardiovascular disease. Hypertension is an indication of cardiovascular issues which should be addressed by a healthcare professional.
The scope of our information is limited to chiropractic and spinal injuries and conditions. To discuss options on the subject matter, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .
By Dr. Alex Jimenez
Additional Topics: Wellness
Overall health and wellness are essential towards maintaining the proper mental and physical balance in the body. From eating a balanced nutrition as well as exercising and participating in physical activities, to sleeping a healthy amount of time on a regular basis, following the best health and wellness tips can ultimately help maintain overall well-being. Eating plenty of fruits and vegetables can go a long way towards helping people become healthy.

TRENDING TOPIC: EXTRA EXTRA: About Chiropractic
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card