Piriformis Treatment
The piriformis muscle (PM) is well-known in medicine as a significant muscle of the posterior hip. It is a muscle that has a role in controlling hip joint rotation and abduction, and it is also a muscle made famous due to its ‘inversion of action’ in rotation. The PM also garners attention due to its role in ‘piriformis syndrome,’ a condition implicated as a potential source of pain and dysfunction.
Piriformis syndrome can be defined as a medical condition in which the piriformis muscle, located in the buttock region, spasms and causes buttock pain. The Sciatic Nerve may be irritated by the interaction between the SN and the PM, producing posterior hip pain down the posterior thigh, imitating ‘sciatica.’
Complaints of buttock pain with the referral of symptoms are not unique to the Piriformis Muscle. Symptoms are widespread with more clinically evident back pain syndromes. It has been indicated that piriformis syndrome is accountable for 5-6 percent of cases of sciatica. In the majority of instances, it happens in middle-aged individuals and is far more prevalent in women.
Table of Contents
Anatomy
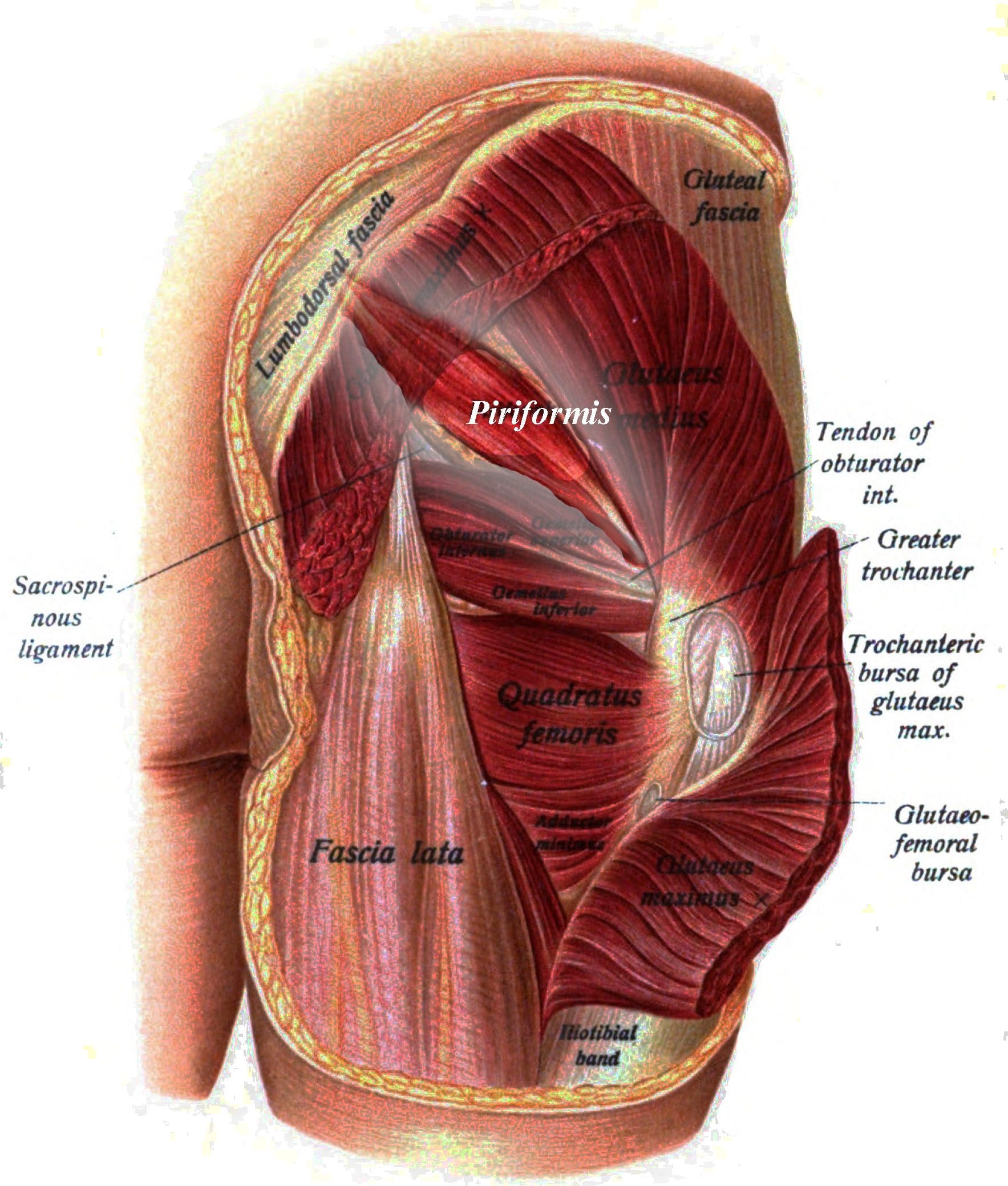 The PM originates on the anterior surface of the sacrum and is anchored to it by three fleshy attachments between the first, second, third, and fourth anterior sacral foramina. Occasionally its origin may be so broad that it joins the sacroiliac joint capsule above and with the sacrotuberous and/or sacrospinous ligament below.
The PM originates on the anterior surface of the sacrum and is anchored to it by three fleshy attachments between the first, second, third, and fourth anterior sacral foramina. Occasionally its origin may be so broad that it joins the sacroiliac joint capsule above and with the sacrotuberous and/or sacrospinous ligament below.
PM is a thick and bulky muscle. As it passes out of the pelvis through the greater sciatic foramen, it divides the foramen into the suprapiriform and infra-piriform foramina. As it courses anterolaterally through the greater sciatic foramen, it tapers out to form a tendon attached to the superior-medial surface of the greater trochanter, commonly blending with the common tendon of the obturator internus and Gemelli’s muscles.
The nerves and blood vessels in the suprapiriform foramen are the superior gluteal nerve and vessels. In the infra-piriformis fossa are the inferior gluteal nerves and vessels and the sciatic nerve (SN). Due to its large volume in the greater sciatic foramen, it can compress the numerous vessels and nerves that exit the pelvis.
PM is closely associated with the other short hip rotators that lie inferior such as the superior gemellus, obturator internus, inferior gemellus, and obturator externus. The primary difference between the PM and other short rotators is the relationship to the SN. The PM passes posterior to the nerve, whereas the other rotators pass anterior.
Causes: Piriformis Syndrome (PS)
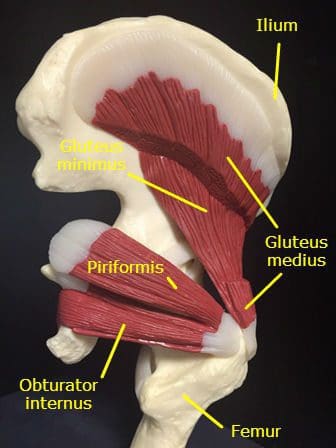 Piriformis Syndrome may be caused by or related to three primary causative factors;
Piriformis Syndrome may be caused by or related to three primary causative factors;
- Tight and shortened muscle fibers precipitated by muscle overuse such as squat and lunge movements in external rotation or direct trauma. This increases the girth of the PM during contraction and may be the source of the compression/entrapment.
- Entrapment of the nerve.
- Sacroiliac Joint Dysfunction (SI Joint Pain) causing PM spasm.
Symptoms
Typical symptoms of piriformis syndrome include:
- A tight or cramping sensation in the buttock and/or hamstring.
- Gluteal pain.
- Calf pain.
- Aggravation from sitting and squatting.
- Peripheral nerve symptoms, i.e., pain and paraesthesia in the back, groin, buttocks, perineum, behind the thigh.
Piriformis Treatment
 When it is believed that piriformis syndrome exists and the clinician feels that a diagnosis has been made, the treatment will usually depend on the suspected cause. If the PM is tight and in spasm, then initially, conservative treatment will focus on stretching and massaging the tight muscle to remove the PM from the pain source.
When it is believed that piriformis syndrome exists and the clinician feels that a diagnosis has been made, the treatment will usually depend on the suspected cause. If the PM is tight and in spasm, then initially, conservative treatment will focus on stretching and massaging the tight muscle to remove the PM from the pain source.
If this fails, then the following has been suggested:
- Local anesthetic block – performed by anesthesiologists who have expertise in pain management.
- Steroid injections into the PM.
- Botulinum injections into the PM.
- Nerve Surgery.
Therapist-directed interventions such as stretching the PM and direct trigger point massage have always been advocated.
Summary
The piriformis muscle is a solid and powerful muscle that runs from the sacrum into the femur. It runs beneath gluteal muscles; the nerve travels beneath them. If this muscle goes into spasm, then the nerve creates radiating pain, numbness, tingling, or burning out of the buttocks to the leg and foot. Other people develop the syndrome while dealing with chronic low back pain.
Activities and motions that cause the piriformis muscle to contract further compress the sciatic nerve, causing pain. This muscle contracts once we squat, or stand, walk, go up steps. It tends to tighten when we sit at any position for more than 20 to 30 minutes.
Individuals with a history of chronic low back pain frequently assume that their radiating sciatic pain is traceable to their lower spine. Their history of disc herniations, or sprains, strains have taught them to assume that it will go away like normal and that the pain is out of their spine. It is just when the pain doesn’t respond as usual that individuals seek therapy, thus delaying their recovery.
Chiropractic Clinic Extra: Physical Rehabilitation & Chiropractic
Post Disclaimer
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Piriformis Treatment" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
📆 Schedule Appointment: Schedule 24/7 (Click Here)

