It’s not unusual for runners to experience tingling, pins and needles, and numbness in their feet while running. Running foot numbness is a relatively common problem for runners and can be easily remedied. Numbness will present in one part of the foot or just the toes. Sometimes it can spread throughout the whole foot. Different causes, most of which are not serious, can be easily dealt with. Serious causes can be treated with chiropractic, massage, decompression therapy, and functional medicine.
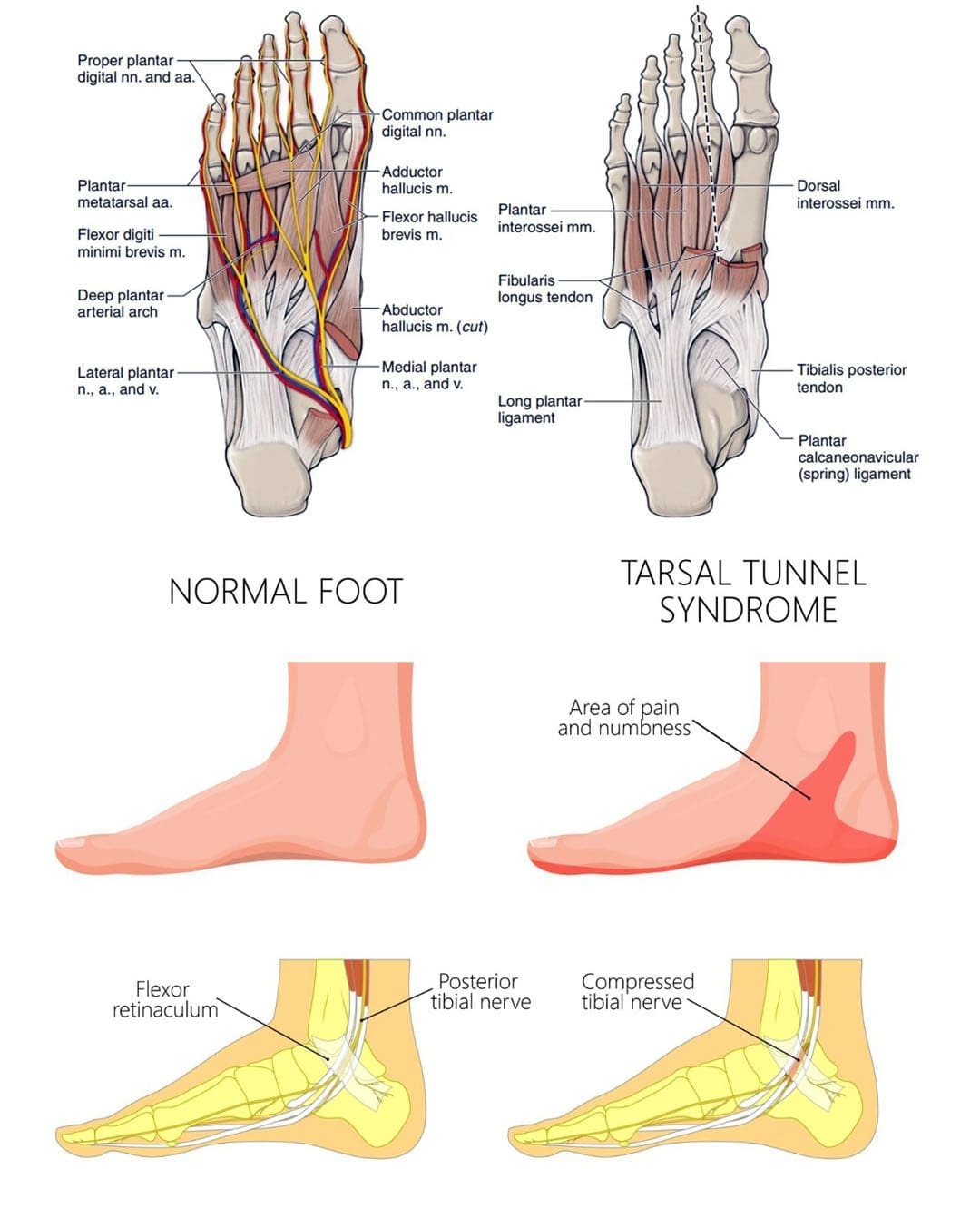
Table of Contents
Running Foot Numbness
Reasons why the feet experience numbing sensations when running, include:
- Improper footwear.
- Laces that are tied too tightly.
- Foot strike pattern.
- Foot structure.
- Training schedule.
- Muscle tightness.
- Compressed nerve.
- Medical conditions like neuromas or peripheral neuropathy.
Footwear
- A common cause of running foot numbness is having overly tight shoes that place added pressure on nerves.
- If this could be the reason, the remedy is to get new shoes.
- Try to find a store that specializes in running shoes and ask for help.
- Footwear professionals look at the size of the foot, the shape, and running gait.
- For example, individuals with a wide foot may need a style with a wider/larger toebox or the front of the shoe that houses the forefoot.
- Get a pair that’s one-half to a full size larger than a regular everyday shoe size.
- This is because when running, the feet swell, especially in hot and humid weather.
- Going up a half or whole size will also accommodate thicker socks for individuals that run in cold weather.
- Sometimes numbness can result from biomechanical issues that can be corrected with the proper shoe.
Tight Laces
- Sometimes it’s not the shoes but the laces that are too tight.
- Pulling a little tighter to get a firm fit around the ankle is common, but this can entrap nerves on top of the foot at the ankle/anterior tarsal tunnel, similar to the carpal tunnel in the wrist.
- This can be problematic for individuals with high arches.
- Loosening the laces are recommended.
- However, runners may feel insecure with looser laces.
- Experimenting with different lacing techniques is recommended to find one that keeps the shoes comfortable without creating undue pressure over the top of the foot.
- Using padding under the tongue of the shoe can help.
Foot Fall Pattern
- Sometimes running form can put pressure on nerves that, lead to numbness.
- Overstriding – Landing heel first with the foot ahead of the body’s center of gravity places the feet on the ground for too long.
- Correcting this issue can be achieved by shortening the stride and focusing on landing on the midsole.
- This way, the feet will land directly under the body.
- Running like stepping on hot coals is recommended, keeping the movements light and quick.
- Correcting overstriding saves energy and lowers the risk of shin splints.
- A sports chiropractor, physical therapist, or running coach can help fine-tune form for specific guidance.
Foot Structure
- The anatomy of the feet, specifically the arches, can contribute to running foot numbness.
- Flat feet mean the entire bottom of each foot is in contact with the floor when barefoot.
- Overly flexible feet are more likely to experience nerve compression.
- This can be corrected with shoe orthotic inserts.
- Over-the-counter orthotics may work, but custom orthotics are another option if they don’t.
Muscle Tightness
- Stiff, inflexible muscles can lead to anatomical conditions that generate nerve pressure.
- Warm-up exercises before running will get the muscles loose and ready.
- Stretching is very important before and after running.
- Individuals prone to muscle tightness should include flexibility exercises.
- Yoga can improve flexibility and body alignment.
- Foam rollers and other massage tools will work out kinks in areas where tightness forms and affects nerves, like the quadriceps, calves, hamstrings, and I.T. band.
- Regular sports massage and chiropractic can help keep the body pliable.
Sciatic Nerve Issues
- A compressed nerve causes a decrease in the sensation to the areas the nerve supplies.
- Foot numbness, especially around the heel or the sole, can be caused by sciatic nerve compression.
- The pain from sciatica might originate in the back but can end up causing numbness in the feet and/or toes.
- Poor posture, tight piriformis muscles, or other back injuries can also cause sciatica.
- A chiropractor or physical therapist can prescribe decompression therapy, MET stretches, and rehabilitative exercises.
Prevention
Most of the time, running foot numbness can be treated by adjusting footwear or technique. Here are a few tips for injury prevention:
Evaluate Shoes
- First, make sure the shoelaces are not overly tight.
- If the shoes are uncomfortable when running, look for another set and get a custom fitting.
Running Form
- Avoid overstriding by focusing on landing on the midsole instead of the heel.
- This will take the pressure off of the feet.
Foot Orthotics
- Individuals with flat feet, high arches, or overly flexible feet should consider orthotics.
Avoid Overtraining
- Work rest days into the training schedule and gradually build up to avoid overuse injuries.
Stretch to prevent muscle imbalances, keep muscles loose, and improve the range of motion.
Chiropractic and Physical Therapy
- If symptoms don’t improve, see a doctor, podiatrist, or chiropractor so they can rule out conditions and develop a personalized treatment plan.
Benefits of Custom Foot Orthotics
References
Aldridge, Tracy. “Diagnosing heel pain in adults.” American family physician vol. 70,2 (2004): 332-8.
Atik, Aziz, and Selahattin Ozyurek. “Flexible flatfoot.” Northern Clinics of Istanbul vol. 1,1 57-64. 3 Aug. 2014, doi:10.14744/nci.2014.29292
Jackson, D L, and B L Haglund. “Tarsal tunnel syndrome in runners.” Sports medicine (Auckland, N.Z.) vol. 13,2 (1992): 146-9. doi:10.2165/00007256-199213020-00010
Souza, Richard B. “An Evidence-Based Videotaped Running Biomechanics Analysis.” Physical Medicine and rehabilitation clinics of North America vol. 27,1 (2016): 217-36. doi:10.1016/j.pmr.2015.08.006
Sridhara, C R, and K L Izzo. “Terminal sensory branches of the superficial peroneal nerve: an entrapment syndrome.” Archives of physical medicine and Rehabilitation vol. 66,11 (1985): 789-91.
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card


