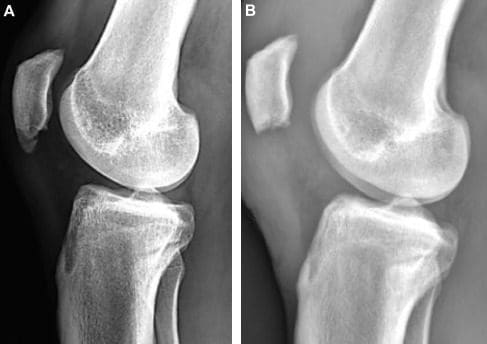
Sinding-Larsen-Johansson, or SLJ, syndrome is a debilitating knee condition that most commonly affects teens during periods of rapid growth. The kneecap, or patella, is attached to the shinbone, or tibia, from the patellar tendon. The tendon connects to an expansion plate at the bottom of the kneecap throughout growth.
Repetitive stress on the patellar tendon can make the growth plate within the knee become inflamed and irritated. SLJ mainly develops in children and adolescents between the ages of 10 and 15 because that is when most people experience growth spurts. SLJ is most common in young athletes due to excess or repetitive strain in the knee.
Table of Contents
Causes of SLJ Syndrome
The large muscle group at the front of the upper leg is known as the quadriceps. When straightening the leg, the quadriceps pull to deliver the leg forward. This puts pressure on the growth plate at the bottom of the kneecap. During rapid growth, the bones and muscles don’t always grow at precisely the same rate.
Since the bones grow, tendons and muscles can get tight and stretched. This increases the strain around the patellar tendon and also on the growth plate it’s attached to. Repetitive or extra stress and pressure in this area can cause the growth plate to become irritated and painful. Matters that can contribute to growing SLJ syndrome are comprised of:
- Sports that involve a lot of running and jumping, such as field and track or other sports such as football, gymnastics, basketball, lacrosse, and field hockey, can place stress on the knees.
- Increased or incorrect physical activity can add strain on the knees. Improper form while training, shoes that don’t support the toes or an unusual way of jogging can increase chances of SLJ syndrome.
- Tight or stiff quadriceps muscles can also lead to SLJ syndrome. Muscles that are more powerful and more elastic will work better, reducing the strain on the patellar and kneecap tendon.
- Activities that place more pressure on the knees or demanding tasks for the knees, such as lifting heavy items, walking up and down stairs, and squatting can cause SLJ syndrome. If there’s already pain on the knee, then these movements may make it worse.
Symptoms of SLJ Syndrome
Symptoms demonstrating the presence of Sinding-Larsen-Johansson, or SLJ, syndrome include: pain at the front of the knee or near the bottom of the kneecap, as this is the main symptom of SLJ; swelling and tenderness around the kneecap; pain that increases with physical activities like jogging, climbing stairs, or leaping; pain that becomes more acute when kneeling or squatting; and a swollen or bony bump at the bottom of the kneecap.

Sinding-Larsen-Johansson, or SLJ, syndrome is medically referred to as a juvenile osteochondrosis which affects the patella tendon in the kneecap which attaches to the inferior pole of the patella in the shinbone. Commonly characterized by knee pain and inflammation, SLJ is considered an overuse knee injury rather than a traumatic injury. Sinding-Larsen-Johansson syndrome is similar to Osgood-Schlatter syndrome.
Dr. Alex Jimenez D.C., C.C.S.T. Insight
Diagnosis of SLJ
Should you see a healthcare professional for knee problems, they will generally ask questions about how much pain the patient is experiencing and if they do any sports or other physical activities and exercises. Whether or not the patient has also had a recent growth spurt, the doctor will examine the patient’s knee for swelling and tenderness.
In very rare instances, the healthcare professional may also ask patients to acquire an X-ray or other imaging diagnostics, such as magnetic resonance imaging, or MRI, to rule out other health issues like fracture or disease.
Prevention of SLJ
The most significant way that patients can prevent getting SLJ is to stop doing physical activities which cause pain in the knee. The patient should limit themselves before the pain goes off.
It is crucial to warm up well and stretch before exercising, playing sports or engaging in any other physical activities. A jog around the track for a couple of minutes and some dynamic stretching is enough to warm up the body.
If the quadriceps muscles are tight, then you might want to do some specialized exercise and physical activity routines. Talk to your healthcare professional, such as a chiropractor or physical therapist, to discuss what’s best for you. Doing a few stretches and warm up exercises after sports or physical activities can help prevent SLJ syndrome from developing.
Treatment of SLJ
The first and most important way to treat SLJ is to stop any action that causes irritation in the knee. It’s essential for a patient to not resume any physical activities without first being cleared by a healthcare professional.
SLJ can be challenging to treat since it may not completely resolve before the bones have completely matured and the growth plates are completely shut. During physical activities, knee pain may come and go in the meantime. Other treatments to help ease SLJ syndrome include:
- Use the RICE formula.
- Rest. Limit physical activities as much as possible and keep weight off the knee. Walking must be kept to a minimum.
- Ice. Apply ice or a cold compress to the affected area for 15 to 20 minutes every few hours. Repeat this for 2 to 3 days or until the painful symptoms have decreased.
- Compress. Give the knee additional support with a strap, a band, or a ribbon. This will also help manage symptoms.
- Elevate. Keep the knee higher than the heart to reduce swelling.
- Take anti-inflammatory or painkilling drugs. Painkillers like acetaminophen and ibuprofen can help relieve pain and decrease swelling.
- Begin a stretching and strengthening program. After the pain and tenderness on your knee have been gone, speak with your physician or sports injury professional about a physical rehabilitation program to strengthen the muscles of your leg and increase their flexibility and range of movement.
It’s easy to become impatient when sidelined by an injury, but the proper treatment can help build the strength needed for future physical activities. The scope of our information is limited to chiropractic as well as to spinal injuries and conditions. To discuss the subject matter, please feel free to ask Dr. Jimenez or contact us at
Curated by Dr. Alex Jimenez

Additional Topic Discussion: Relieving Knee Pain without Surgery
Knee pain is a well-known symptom which can occur due to a variety of knee injuries and/or conditions, including sports injuries. The knee is one of the most complex joints in the human body as it is made-up of the intersection of four bones, four ligaments, various tendons, two menisci, and cartilage. According to the American Academy of Family Physicians, the most common causes of knee pain include patellar subluxation, patellar tendinitis or jumper’s knee, and Osgood-Schlatter disease. Although knee pain is most likely to occur in people over 60 years old, knee pain can also occur in children and adolescents. Knee pain can be treated at home following the RICE methods, however, severe knee injuries may require immediate medical attention, including chiropractic care.

EXTRA EXTRA | IMPORTANT TOPIC: Recommended El Paso, TX Chiropractor
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card