There are several important factors to consider, such as when an MRI scan must be performed and limitations with an interpretation of findings to get an MRI scan for herniated discs.
To begin with, the difficulty with the results of an MRI scan, as with several other diagnostic studies, is that the abnormality may not always be the source of an individual’s back pain or other symptoms. Numerous studies have shown that approximately 30 percent of people in their twenties and forties have a lumbar disc herniation in their MRI scan, even though they don’t have any pain.
An MRI scan cannot be interpreted on its own. Everything Has to Be well-correlated to the individual patient’s condition, for example:
- Symptoms (such as the duration, location, and severity of pain)
- Any deficits in their examination
Another concern with MRI scans is the time when the scan is done. When a patient has experienced the following symptoms would be the only time that an MRI scan is needed immediately:
- Bowel or bladder incontinence
- Progressive weakness due to nerve damage in the legs.
Table of Contents
Herniated Disc Analysis with MRI
Obtaining an MRI (magnetic resonance imaging) can be important in correctly assessing a herniated disc in the spine. Unlike an X-ray, MRI uses a magnetic field and a computer to create and record detailed pictures of the internal workings of your entire body. This technology can also produce cross-sectional views in identifying a disc of the body, which greatly helps doctors. MRI scans are based on new technology, but they have become essential in diagnosing several back and neck issues, such as spinal stenosis, herniated discs, and bone spurs.
An MRI scan has several benefits that greatly help a herniated disc patient. The advantages of an MRI can be:
- Unobtrusive
- Painless and free of radiation
- Can focus on a particular part of the entire body
- Extremely accurate
Diagnosing Disc Herniation
Should you believe you have a herniated disc in the neck or back, the very first step would be to visit a physician. Your physician can supply you with a complete evaluation and inspection of your medical history to create an identification. Following that, you may be referred to execute an MRI to stabilize and confirm the herniated disc.
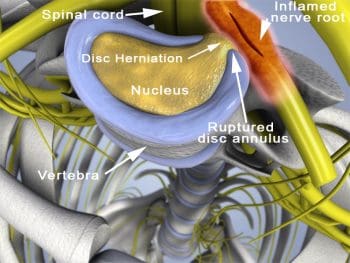
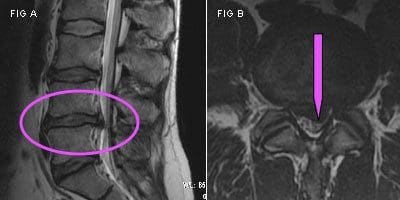
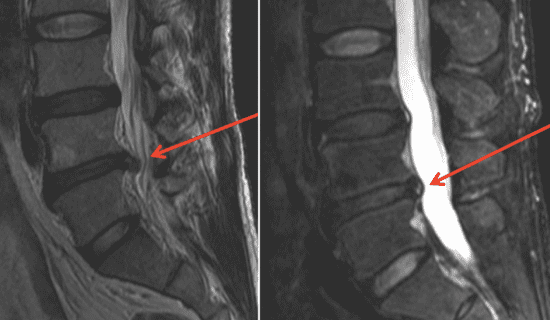
You’ll be put into the tubular MRI machine at the imaging center to get a body scan. You may remain enclosed in the MRI device for up to an hour while the comprehensive scan of the place where the herniated disc along the spine is completed. The MRI can reveal the exact condition of the herniated disc and surrounding arrangements. This allows your doctor to produce the right treatment plan for you and understand the origin of the disc damage and pain.
Herniated Disc Follow-Up Treatment
Most patients can successfully treat herniated disc pain using nonsurgical standard treatments prescribed by their physician. These include relaxation, compression treatment, and mild exercise. Surgery can then be explored when months or weeks of treatment do not bring a return to the previous action.
Contact a specialist if you’re researching surgical options and have become concerned by several of the risks and unsuccessful results of traditional open-back operations. Spine surgery specialists perform minimally invasive spine surgery, including invasive stabilization surgeries and minimally invasive decompression, which can treat several acute herniated discs. They may review your MRI to determine if you are a candidate for minimally invasive spine surgery, which may help you regain your life.
Additional Topics: Sciatica
Lower back pain is one of the most commonly reported symptoms among the general population. Sciatica is a well-known group of symptoms, including lower back pain, numbness, and tingling sensations, which often describe the source of an individual’s lumbar spine issues. Sciatica can be due to various injuries and/or conditions, such as spinal misalignment or subluxation, disc herniation, and spinal degeneration.
Post Disclaimer
Professional Scope of Practice *
The information herein on "MRI for Herniated Disc Diagnosis" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Our information scope is limited to Chiropractic, musculoskeletal, acupuncture, physical medicines, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somatovisceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and/or functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez, DC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, RN*, CCST, IFMCP*, CIFM*, ATN*
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807, New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Florida
Florida License RN License # RN9617241 (Control No. 3558029)
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Presently Matriculated: ICHS: MSN* FNP (Family Nurse Practitioner Program)
Dr. Alex Jimenez DC, MSACP, RN* CIFM*, IFMCP*, ATN*, CCST
My Digital Business Card


 Again We Welcome You¸
Again We Welcome You¸
