Table of Contents
Do you feel:
- Hormone imbalances?
- Excessively foul-smelling sweat?
- Excessive belching, burping, or bloating?
- Digestive problems subside with relaxation?
- Difficult bowel movement?
If you are experiencing any of these situations, then you might be experiencing some gut and liver issues in your body.
The role of the gut-liver axis in NAFLD (non-alcoholic fatty liver disease) has been examining probiotics and have found some new information on the gut microbiome and how probiotics work in NAFLD. The new information that future research found was quite interesting. It stated that there were about 26 major randomized controlled trials that used probiotics for NALFD that ranged between 20 to 200 individuals in four weeks to 1 year. The laboratory assessments included liver enzymes and anthropometric parameters in the body. Some of the studies added cardiovascular risk factors like C-reactive proteins and lipid profiles as markers for insulin resistance. Furthermore, most of the studies have used a probiotic formulation that includes multiple species, although a few were conducted by using a single strain.
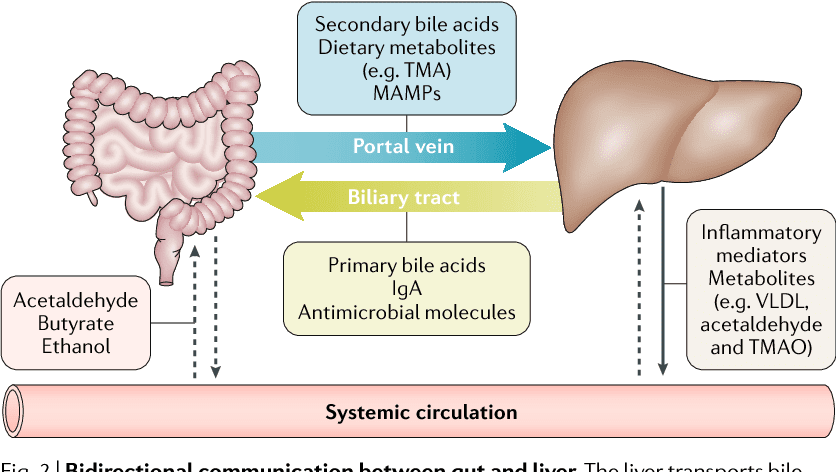
What NAFLD does to the body is that it becomes a hepatic consequence of metabolic syndrome. This includes obesity, diabetes, and dyslipidemia. What is interesting about the connection between gut microbiota and NAFLD has been attracting a significant amount of attention in recent years. The data has shown that the gut microbiota can affect the hepatic lipid metabolism while also influencing the balance between pro/anti-inflammatory effectors in the liver.
Chronic Liver Diseases
Even though chronic liver disease is the primary cause of morbidity and mortality worldwide. Studies showed that gut dysbiosis was identified as an essential factor in the pathogenesis of the liver disease. The relationship between the gut microbiota and the liver is still not understood, but the dysfunction of leaky gut and an increased bacterial translocation into the liver. Another study showed that immense importance is a massive advancement in understanding the roles of the gut and liver microbiome that is driven by a high DNA sequencing and improving them.
There are many stages of liver disease that can happen, but when it comes to excessive alcohol in the liver. Studies show that excessive alcohol consumption is the leading cause of chronic liver disease worldwide. The stages of alcoholic liver disease are hepatic steatosis, steatohepatitis, and, ultimately, liver cirrhosis. One of the main characteristics of alcohol liver disease is that there is an increased gut permeability due to a direct toxic effect of alcohol on the epithelial cell in the gastrointestinal tract and a decreases expression of the tight-junction protein.
Probiotic Supplements
For probiotic supplementation, they have demonstrated a significant decrease in liver enzymes, which were compared to the placebo group. Studies found that probiotics were shown to have synergistic effects with metformin on liver enzymes for patients that have NASH. Any products that contained both prebiotics and probiotics can demonstrate a similar effect in the probiotic groups. In another study, it showed a reduction of intrahepatic fat that is measured by MRI, but the improvement in liver enzymes in the body did not reach any clinical significance. It is essential to know that liver enzymes can have a highly variable and do not always have a direct correlation with disease progression that they may encounter.
Research shows that there are five meta-analyses included and that they all demonstrated that probiotics and synbiotics have improved on AST and ALT levels in the body significantly. Surprisingly, several other studies have assisted probiotics by countering hepatic steatosis, fibrosis, and liver stiffness in the body. Ultrasound imaging can help assist these parameters and show some positive clinical outcomes with these two supplements.
When probiotics help restore the gastrointestinal barrier function in the body, they can eliminate the harmful bacteria that has interacted with the gastrointestinal system. Not only that, but probiotics can also be beneficial by modulating the immune system, reduce liver fats, and improve the liver enzymes as well. By using probiotics, they are most likely to be more productive by helping the body and preventing bacterial translocation in the gut, thus reducing the effects of the intestinal microbiota on the liver to prevent chronic illnesses from forming and causing havoc.
Conclusion
For individuals that have NAFLD, they will already establish the disease and required a higher nutrient intake demand than what can be obtained from any diets alone. So using dietary supplements should be considered to help reduce the NAFLD disease’s progression, thus improving the liver and its functions. The gut-liver axis is connected to the body since if anything happens to the liver like chronic diseases, it can affect the gut as well. Using probiotics to help the liver is essential to make sure that the liver is functioning correctly and that the body is being as healthy as possible. Some products are here to offer gastrointestinal and metabolic support while also supporting multiple aspects of the biliary system.
The scope of our information is limited to chiropractic, musculoskeletal, and nervous health issues or functional medicine articles, topics, and discussions. We use functional health protocols to treat injuries or disorders of the musculoskeletal system. Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. To further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900.
References:
Jurgelewicz, Michael. “New Review Demonstrates the Role of the Gut Microbiome and Probiotics in Nonalcoholic Fatty Liver Disease.” Designs for Health, 25 Nov. 2019, blog.designsforhealth.com/node/1160.
Konturek, Peter Christopher, et al. “Gut?Liver Axis: How Do Gut Bacteria Influence the Liver?” Medical Sciences (Basel, Switzerland), MDPI, 17 Sept. 2018, www.ncbi.nlm.nih.gov/pmc/articles/PMC6165386/.
Tripathi, Anupriya, et al. “The Gut-Liver Axis and the Intersection with the Microbiome.” Nature Reviews. Gastroenterology & Hepatology, U.S. National Library of Medicine, July 2018, www.ncbi.nlm.nih.gov/pmc/articles/PMC6319369/.
Xie, Chencheng, and Dina Halegoua DeMarzio. “Role of Probiotics in Nonalcoholic Fatty Liver Disease: Does Gut Microbiota Matter?” MDPI, Multidisciplinary Digital Publishing Institute, 19 Nov. 2019, www.mdpi.com/2072-6643/11/11/2837.
Post Disclaimer
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "The Gut-Liver Connection" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
📆 Schedule Appointment: Schedule 24/7 (Click Here)


