The usage of integrated functional medicine is essential when it comes to our bodies overall health. Local practitioners and health coaches, talk with patients on what seems to bother them. Sometimes it is a simple adjustment, but mostly it’s what’s causing them problems on the inside. Some patients have inflammation around their intestinal epithelial barriers, and it can cause a leaky gut.
In the previous article, we talked about what the microbiomes do in our intestines and what is their functions are in the intestinal epithelial barrier. However, today we will discuss what the immunoglobulins antibodies do with proteins and peptides in the intestinal permeability. As well as explaining what the Lectin Zoomer and the Dairy Zoomer does when a patient has a food sensitivity and needs testing in a two-part series about the intestinal permeability and food zoomers.
Table of Contents
Immunoglobulins
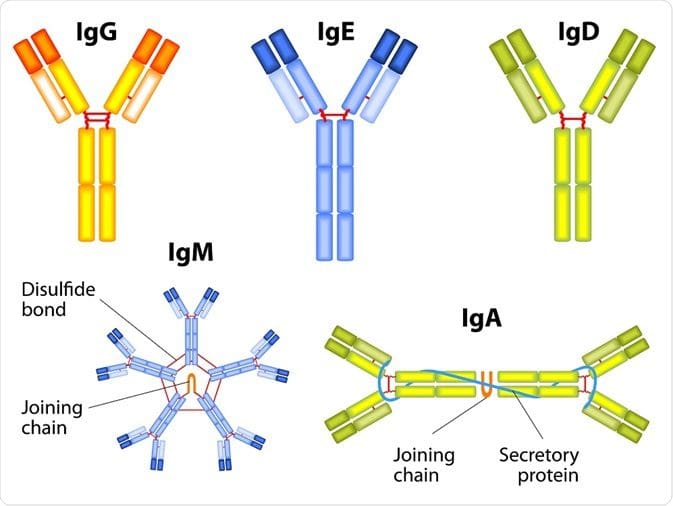
The first thing that we need to know is that immunoglobulins are immune-mediated reactions. So anything that involves the immune system will cause a hypersensitivity reaction to one or more food or foreign proteins, and their presence can be of one or more types of immunoglobulins.
There are 3 terms of hypersensitivities that can be involved with immunoglobulins:
- Allergies are the ones that are most common and are associated with anaphylaxis. Patients can have a very severe and acute immediate reaction to specific allergens like food or environmental like pollen or a bee sting.
- Non-allergies, sensitivity reactions involved either chemical mediators or antibody reactions.
- Food intolerances are non-immune-mediated reactions, and a good example is Lactose Intolerance or a bile salt deficiency. These can make somebody who has a food intolerance, can’t digest fat.
These three terms are often mistaken and used interchangeably clinically, but they are entirely different since they are not interchangeable. Especially when it comes to sensitivities and intolerances because those two commonly get used in place of each other, but they are totally different.
If you are testing your patient’s immunoglobulins, remember that antibodies are particular to each type of foreign substances and can be in three types of hypersensitivity. Antibodies will only bind an react to the specific proteins of the foreign material but not to the substance’s extract. The most common ones are type 3, where it involves IgG, IgA, and IgM. This type can tell us what cells and mechanisms are involved.
Type 3 Hypersensitivity Mechanisms
Here are the types of mechanisms that are involved with Type 3 immunoglobulins.
- Antigens are a foreign protein that is present and is recognized as a threat or non-self.
- Antibodies will bind to the antigen to neutralize or keep it from linking to anywhere else in the body. This is where the immune complex is formed.
- Immune complexes insert themselves into the small blood vessel, joints, tissues, and glomeruli, causing symptoms to the body.
- They are far more capable of interacting with complement proteins to form medium-sized complexes; which has an excess amount of antigens that are high pathogenic.
- However, once the immune complex is in the tissue, it can induce an inflammatory response and cause damage to the body. This damage is the result of the action of cleaved complement anaphylatoxins, which can mediate a mast cell degranulation.
- With the recruitment of inflammatory cells in the tissue, it can lead to tissue damage through phagocytosis.
IgA and IgG
In a previous article, we mentioned the mechanics of the intestinal permeability. However, we going to discuss what IgA antibodies and IgG antibodies do to the gut and to the entire body.
IgA Antibodies
IgA antibodies are found in the body where there is a mucosal lining around the areas like the nose, breathing passages, digestive tract, ears, eyes, and vaginal region. These surfaces are exposed to the outside of the environment either by air, food, or other foreign substances regularly.
IgA antibodies actually protect the body surfaces that are exposed to outside foreign substances, and these antibodies can be found in saliva, tears, and blood.
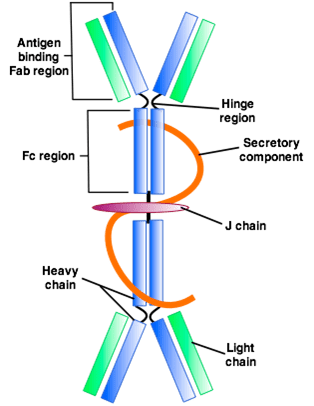
In the gut, however, it can bind to the mucosal layer on the top of the intestinal epithelial cells to form a barrier to neutralizing threats before they reach the cell. And that is very important, especially since IgA is like an insurance policy for your gut.
IgA antibodies are considered as non-inflammatory. Which means that they don’t stimulate inflammatory processes in the body like IgG does. They do, however, create a mucosal response to a foreign antigen, and it is usually microbial (ex., bacteria, yeast, viruses, parasites) or microbial toxins. They can also generate a response to pollutants, toxins, and recognized undigested food as a foreign protein.
In the intestinal lumen, IgA can be indicative of an immune response stimulated by T-b cell interaction. So a healing intervention, if a patient has an abundance of IgA antibodies may need to target TH1 and TH2 balance so it can regulate T-reg production.
IgG Antibodies
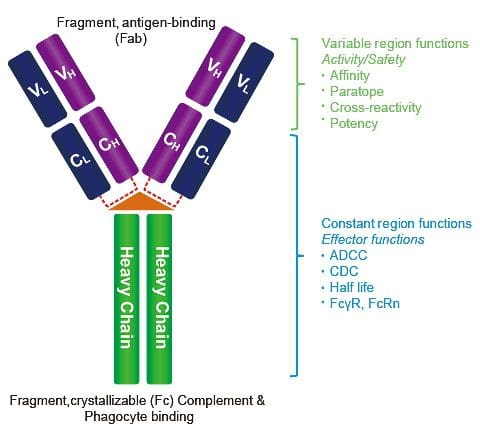
IgG antibodies are found in all body fluids. They happen to be the smallest but the most common of all antibodies as they make-ups about 75% to 80% of antibodies found throughout the entire body. These antibodies are essential as they fight against bacterial and viral infections, and they are the only type that can cross the placenta.
They do indicate exposure to a specific antigen, but they don’t always necessarily indicate active inflammation; however, they can contribute to it in a dose-independent.
Why measure IgA and IgG?
So why do we measure IgA and IgG? Surprisingly some people don’t produce as much or any IgA antibodies, and therefore, local practitioners would not know if their patients have formed a reactivity to an antigen if they don’t check their IgG levels.
Surprisingly, some IgG antibodies are not an indicator of actual inflammation or disease process. Some IgG antibodies are formed in response to a protein as sort of a tracker in the body but do not elicit a reaction. However, IgA antibody is coupled with IgG to indicate a bit stronger immune response to an antigen in some cases.
IgA and IgG in the Protein Level
IgA and IgG testing in the protein level is what the food sensitivity tests are looking at. They look for the whole protein, which is the extract level. All food sensitivity test looks for residues of carbohydrate and lipid-based particles. It’s not pure protein but that what the test does, it seems for the reactive compound. Some of the strengths are that the test gives an acute measure of IgG and IgA to a specific protein. It can also be suitable for associating Type 3 reactions involving IgG and IgA complexes, and if the IgG is pathogenic, then it will be beneficial.
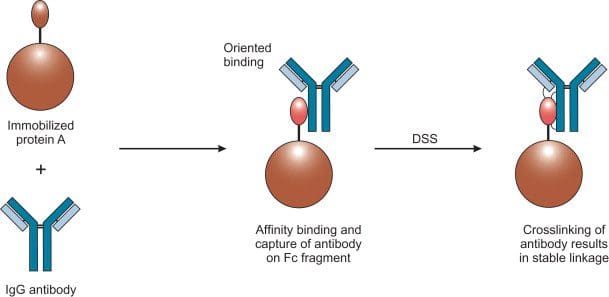
Some of the weaknesses are that IgG can be a protective antibody, and it may be a good thing. It means that the immune system is handling it and there’s nothing necessarily wrong about that. IgG and IgA antibodies represent whole proteins being presented to the immune system can it also be an indicator that a patient may have a lack of sufficient digestive capacity when many food sensitivities are being detected.
IgG and IgA in the Peptide Level
When IgG and IgA are being tested at the peptide level, this is where the food zoomer test focuses on. This is because there is a high level of antibodies specificity, cross-reactivity is minimized if not completely eliminated. The concept of foods that are cross-react, for example, gluten, might cross-react to other foods that are similarly shaped in their molecular structure, then you should eliminate the gluten out of your diet as well as the foods that are in contact with them.
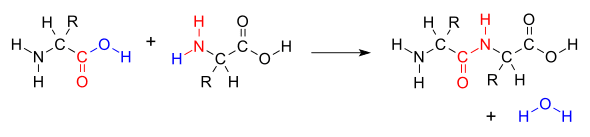
However, if the antibodies to gluten are being picked up at the peptide level, then it won’t look at those foods that are being cross-reactive to gluten. The antibodies will only bind to the individual peptides than the whole protein. This will be a more accurate assessment of whether or not that the patient is sensitive to the foods their body is reacting to.
What is Loss of Oral Tolerance?
Loss of oral tolerance is a term used to describe the phenomenon of someone developing a sensitivity, whether it is accompanied by symptoms or not, and it’s usually a commonly consumed or semi-regularly consumed food. When that happens, there is a production of inflammatory cytokines and antibodies that will respond to the continued exposure to the food.
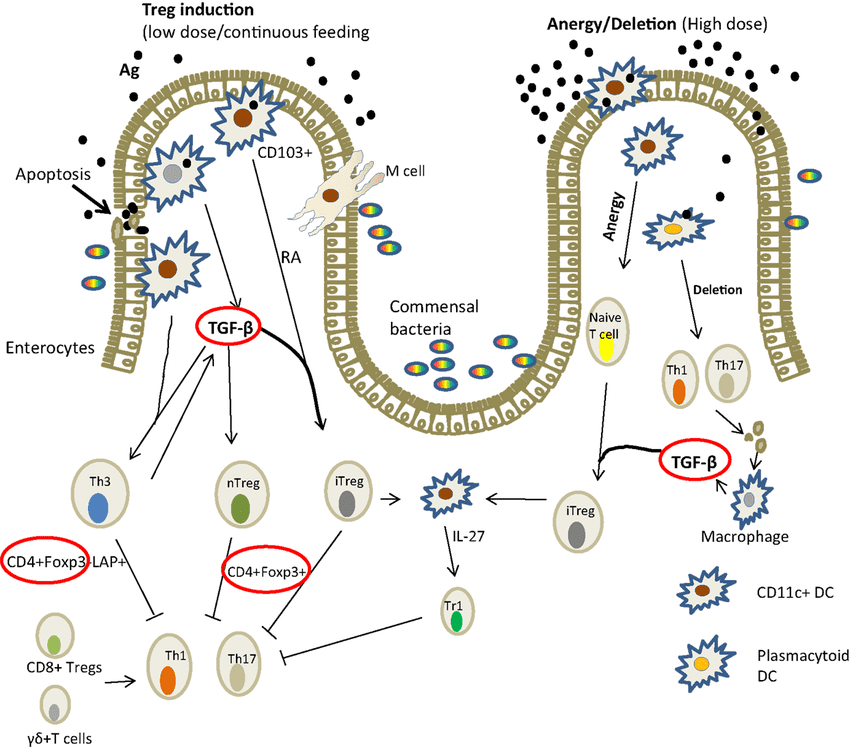
For the inflammatory responses to be eliminated, patients have to remove the offending food for about 3 to 4 weeks if IgA antibodies are present or 3 to 6 months if the IgG antibodies are present as well. This is the only way for the antibodies to disappear, and the intestinal permeability can heal. But the disappearance of antibodies does not guarantee that oral tolerance has been established. If you are retesting a patient and if the antibodies are gone, that indicates that the patient has done an excellent job in eliminating that food from their diet. However, the only way to know is to reintroduce the food and retest after a few months, just to make sure that no antibodies are being produced after the intestinal barrier has been fully healed.
Conclusion
All in all, that is what the intestinal permeability does when we have IgA and IgG antibodies and what do they do when there is food sensitivity in the body. However, it is crucial that our patients understand that we here at Injury Medical Clinic, take the time to study what causes inflammation in our patients and using integrated functional medicine to make sure that their intestines are being healed naturally. In the next article, we will discuss the difference between peptides and proteins, and about the Lectin and Dairy Zoomer.
Post Disclaimer
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Intestinal Permeability and Functional Integrated Medicine Part: 1 El Paso, Texas" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933


