Many types of arthritis can affect the structure and function of the muscles, bones and/or joints, causing symptoms such
Table of Contents
Abstract
Spinal involvement is frequent in rheumatoid arthritis (RA) and seronegative spondyloarthritides (SpA), and its diagnosis is important. Thus, MRI and CT are increasingly used, although radiography is the recommended initial examination. The purpose of this review is to present the typical radiographic features of spinal changes in RA and SpA in addition to the advantages of MRI and CT, respectively. RA changes are usually located in the cervical spine and can result in serious joint instability. Subluxation is diagnosed by radiography, but supplementary MRI and/or CT is always indicated to visualize the spinal cord and canal in patients with vertical subluxation, neck pain and/or neurological symptoms. SpA may involve all parts of the spine. Ankylosing spondylitis is the most frequent form of SpA and has rather characteristic radiographic features. In early stages, it is characterized by vertebral squaring and condensation of vertebral corners, in later stages by slim ossifications between vertebral bodies, vertebral fusion, arthritis/ankylosis of apophyseal joints and ligamentous ossification causing spinal stiffness. The imaging features of the other forms of SpA can vary, but voluminous paravertebral ossifications often occur in psoriatic SpA. MRI can detect signs of active inflammation as well as chronic structural changes; CT is valuable for detecting a
Keywords: Spine, Arthritis, Rheumatoid Arthritis, Spondyloarthropathies
Introduction
The spine can be involved in most inflammatory disorders encompassing rheumatoid arthritis (RA), seronegative spondyloarthritides (SpA), juvenile arthritides and less frequent disorders such as, arthro-osteitis and SAPHO (synovitis, acne, pustulosis, hyperostosis, osteitis) syndrome.
During the last decade, the diagnostic use of magnetic resonance imaging (MRI) and computed tomography (CT) has increased considerably, although radiography is still the recommended initial examination. It is therefore important to know the characteristic radiographic findings in arthritides in addition to the advantages of supplementary MRI and CT. This review will focus on the different imaging features and be concentrated on the most frequent inflammatory spinal changes seen in RA and SpA, respectively. These two entities display somewhat different imaging features, which are important to recognize.

Rheumatoid arthritis is an autoimmune disease which causes the human body’s own immune system to attack and often destroy the lining of the joints. Although it commonly affects the small joints of the hands and feet, rheumatoid arthritis, or RA, can affect any joint in the human body. The neck, or cervical spine, can be affected more often than the lower back if rheumatoid arthritis affects the joints in the spine.
Dr. Alex Jimenez D.C., C.C.S.T.
Rheumatoid Arthritis
Involvement in RA is usually located in the cervical spine where erosive changes are predominantly seen in the
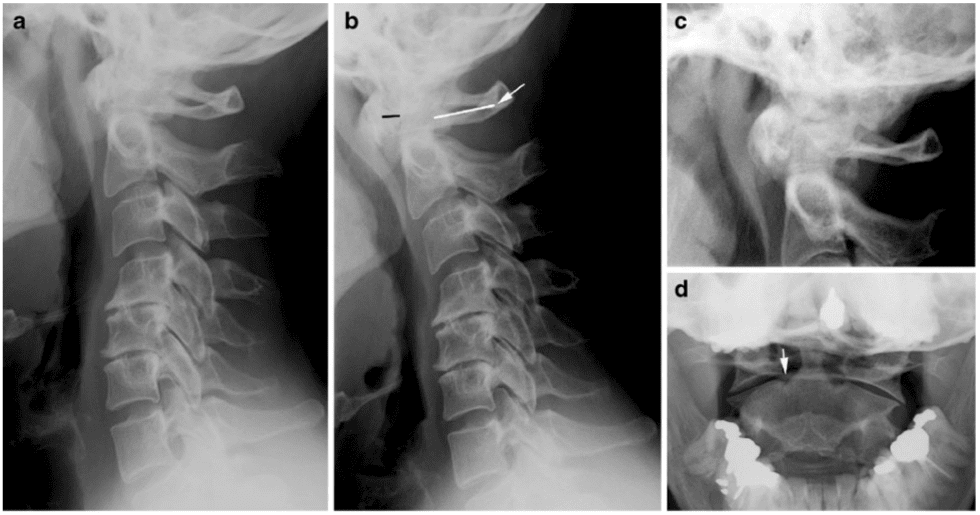
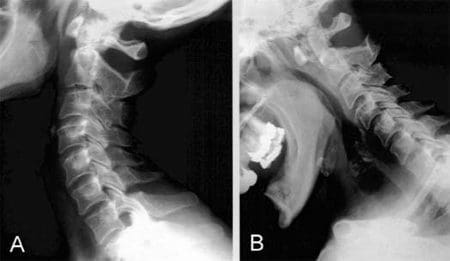
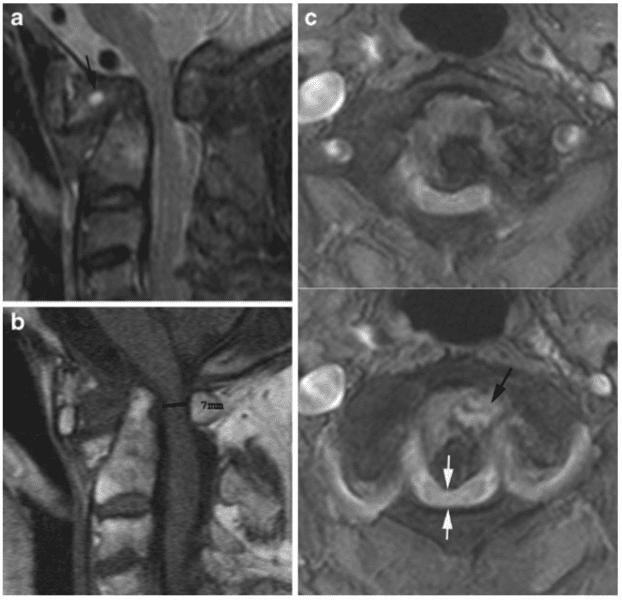
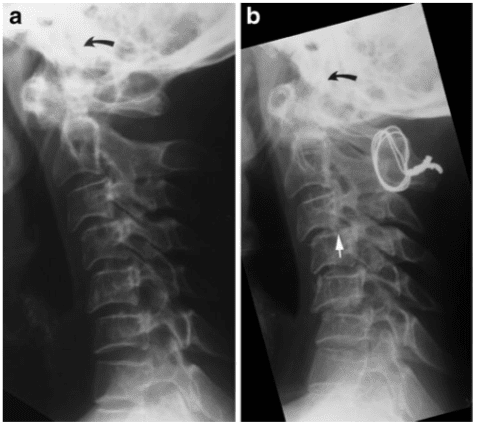
Radiography of the cervical spine is mandatory in RA patients with neck pain [3]. It should always include a lateral view in a flexed position compared with a neutral position in addition to special views of the dens area to detect any lesions and/or instability (Fig. 1). A supplementary lateral view during extension can be useful to assess reducibility of
Anterior
Anterior atlanto-axial subluxation.
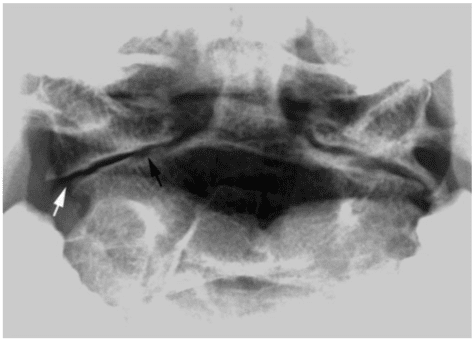
Lateral and rotatory atlanto-axial subluxation. Displacement of the lateral masses of the atlas more than 2 mm in relation to that of the axis and asymmetry of the lateral masses relative to the dens, respectively (Fig. 2). Rotatory and lateral subluxation is diagnosed on open-mouth anterior-posterior (AP) radiographs. Anterior subluxation often coexists because of the close anatomical relation between the atlas and the axis.
Posterior atlanto-axial subluxation. The anterior arc of the atlas moves over the odontoid process. This is rarely
Vertical atlanto-axial subluxation is also referred to as
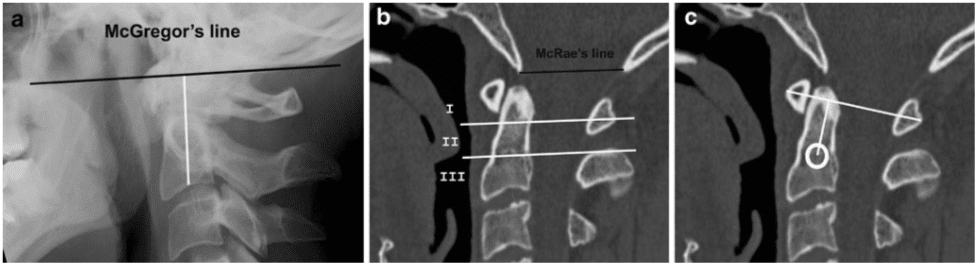

The occurrence of dens erosion can, however, make this measurement difficult to obtain. The Redlund-Johnell method is therefore based on the minimum distance between McGregor’s line and the midpoint of the inferior margin of the body of the axis on a lateral radiograph in a neutral position (Fig. 3) [4]. Visualisation of the palate may not always be obtained. Methods without dens and/or the palate as landmarks have therefore been introduced [4]. The method described by Clark et al. (described in [4]) includes assessment of the location of the atlas by dividing the axis into three equal portions on a lateral radiograph. Location of the anterior
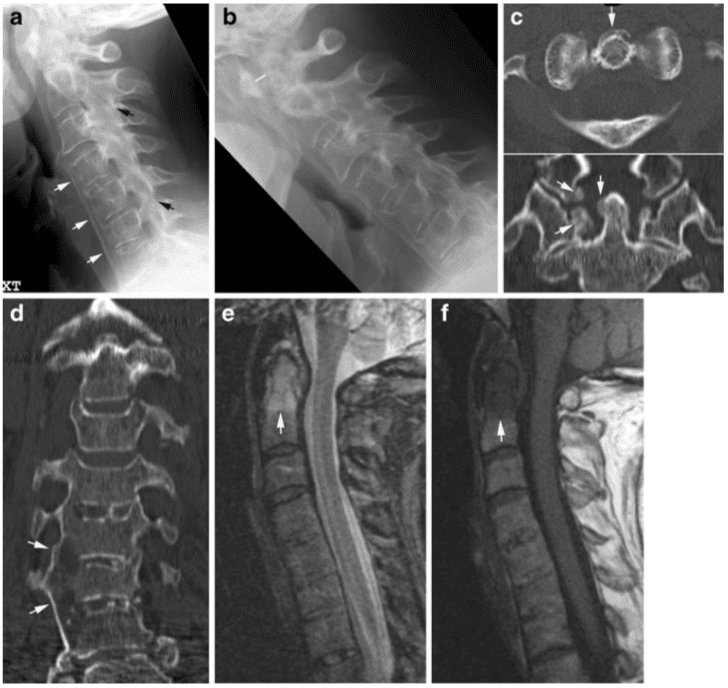
Subaxial RA changes also occur in the form of arthritis of the apophyseal and/or uncovertebral joints, appearing as narrowing and superficial erosions by radiography. It can cause instability in the C2-Th1 region, which is mainly seen in patients with severe chronic peripheral arthritis. Anterior subluxation is far more frequent than posterior subluxation. It is defined as at least 3 mm forward slippage of a vertebra relative to the underlying vertebra by radiography including a flexion view (Fig. 6). Changes are particularly characteristic at the C3–4 and C4–5 level, but multiple levels may be involved, producing a typical “stepladder” appearance on lateral radiographs. The condition is serious if the
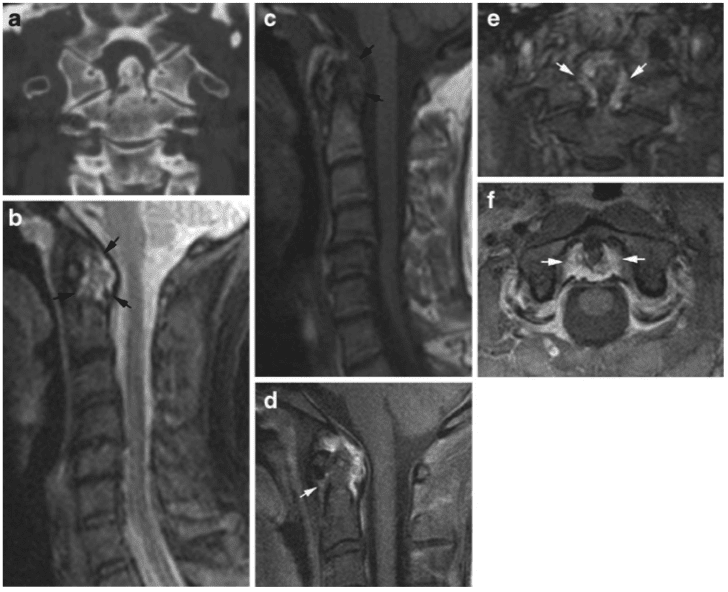
Discitis-like changes and spinous process erosion may also be detected by radiography in RA, but are relatively rare, whereas concomitant degenerative changes occur occasionally (Fig. 1).
Cross-sectional imaging in the form of CT and MRI eliminates
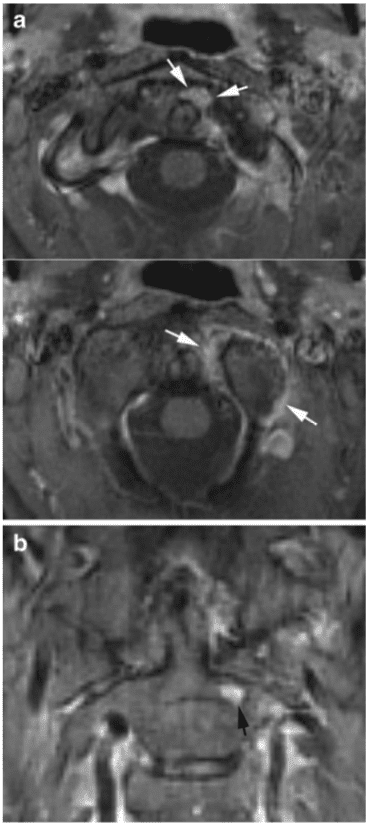
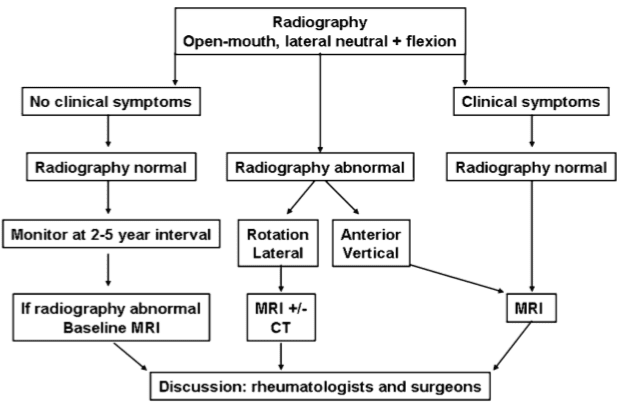
A diagnostic strategy according to Younes et al. [3] is recommended (Fig. 9). This includes an indication for radiography in all RA patients with disease duration >2 years as cervical involvement may occur in over 70% of patients and has been reported to be asymptomatic in 17% of RA patients. It is recommended to monitor patients with manifest peripheral erosions accompanied by RF (rheumatoid factor) and antiCCP (antibodies to cyclic citrullinated peptide) positivity every second year and patients with few peripheral erosions and RF negativity at 5-year intervals. MRI is indicated in patients with neurological deficit, radiographic instability, vertical subluxation and
Seronegative Spondyloarthritides
According to European classification criteria [8, 9], SpA is divided
Ankylosing Spondylitis
Ankylosing spondylitis is the most frequent and usually the most disabling form of SpA. It has a genetic predisposition in the form of a frequent association with the human leukocyte antigen (HLA) B27 [10]. AS often starts in early adulthood and has a chronic progressive course. It is therefore important to diagnose this disorder. According to the modified New York Criteria [11], the diagnosis of definite AS requires the following: manifest sacroiliitis by radiography (grade ?2 bilateral or unilateral grade 3–4 sacroiliitis; Fig. 10) and at least one of the following clinical criteria: (1) low back pain and stiffness for more than 3 months improving with activity, (2) limited movement of the lumbar spine and (3) reduced chest expansion. These criteria are still used in the diagnosis of AS despite the increasing use of MRI to detect the disease early. It is therefore important to know both the characteristic radiographic features and the MR features of AS.
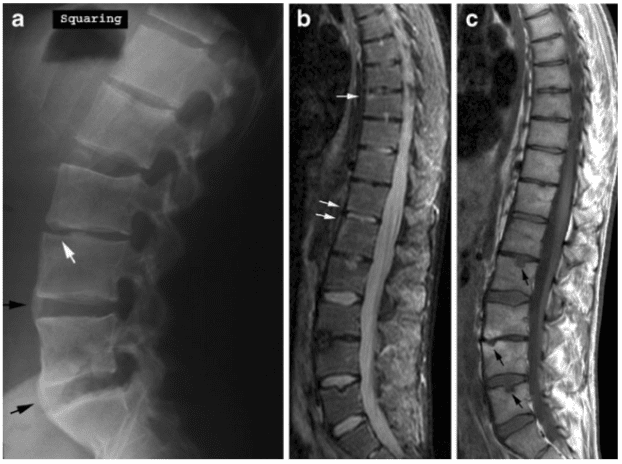
Early radiographic spinal changes encompass erosion of vertebral corners (Romanus lesions) causing vertebral squaring and eliciting reactive sclerosis appearing as condensation of vertebral corners (shiny corners; Fig. 10). These changes are caused by inflammation at the insertion of the annulus fibrosus (enthesitis) at vertebral corners provoking reactive bone formation [12]. Later
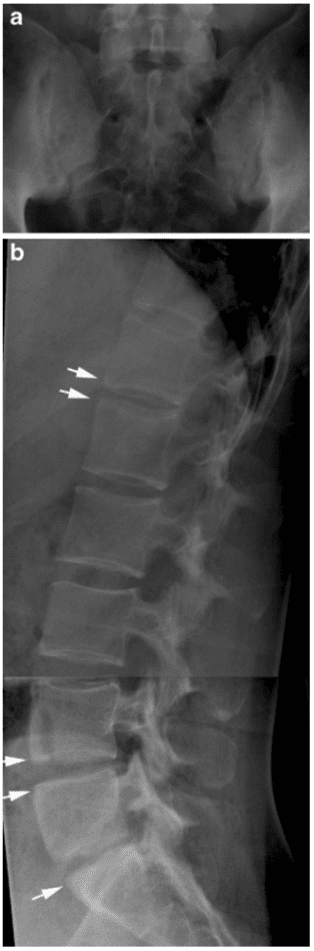
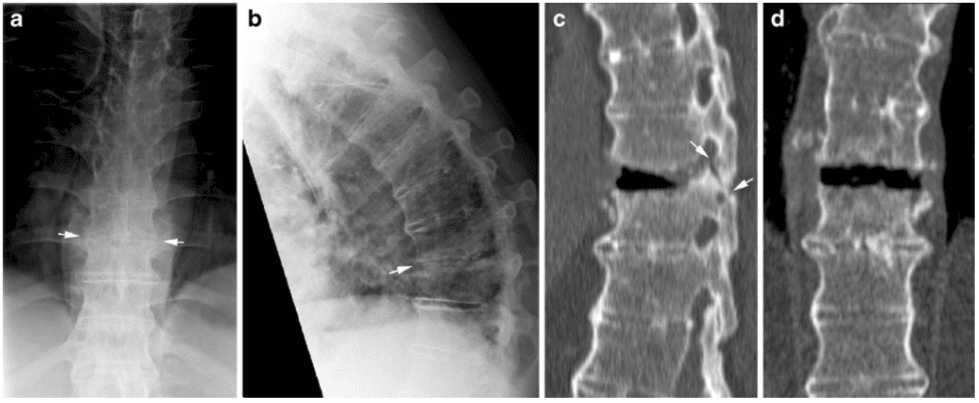
Erosive changes within intervertebral spaces (Andersson lesions) have been detected by radiography in approximately 5% of patients with AS [14], but more frequently by MRI (Fig. 11) [15].
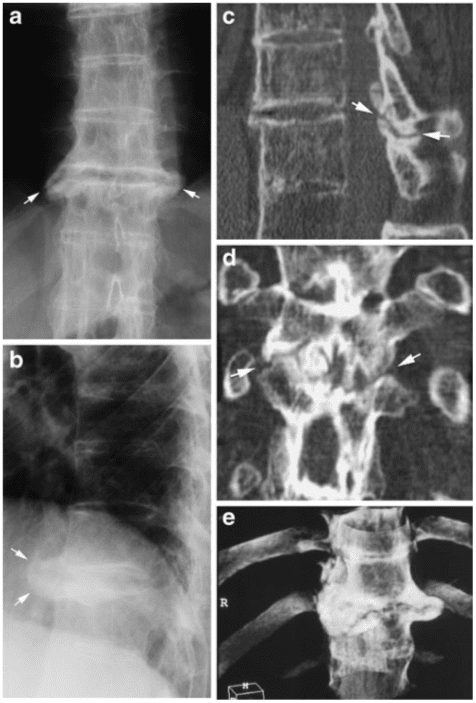
Persistent movement at single intervertebral spaces may occur in an otherwise ankylosed spine, sometimes caused by non-diagnosed fractures. This can result in pseudo- arthrosis-like changes with the formation of surrounding reactive osteophytes due to excessive mechanical load at single movable intervertebral spaces [14]. The diagnosis of such changes may require a CT examination to obtain adequate visualization (Fig. 13).
One of the life-threatening complications of AS is
Cross-sectional CT or MR imaging can be advantageous in the diagnosis of AS changes. CT providing a clear delineation of osseous structures is the preferred technique for visualizing pseudo-arthrosis and detecting fractures (Figs. 13, 14). CT is superior to MRI in detecting minor osseous lesions such as erosion and ankylosis of the apophyseal,
Characteristic MR findings early in the disease are activity changes mainly consisting of
During the disease course signs of activity can also occur at syndesmophytes, apophyseal joints and interspinous ligaments (Fig. 16). Detection of inflammation at apophyseal joints by MRI, however, demands pronounced involvement histopathologically [19]. The inflammation at vertebral corners is the most valid feature and has been observed related to the development of syndesmophytes by radiography [12], establishing a link between signs of disease activity and chronic structural changes.
Chronic AS changes detectable by MRI mainly consist of fatty marrow deposition at vertebral corners (Fig. 17), erosion (Fig. 11) and vertebral fusion in advanced disease (Fig. 12). Fatty marrow deposition seems to be an a sign of chronicity being significantly correlated with radiographic changes, in particular, vertebral squaring [15]. Erosions are more frequently detected by MRI than by radiography (Fig. 11) [15] and can present with signs of active inflammation and/or surrounding fatty marrow deposition compatible with sequels of osseous inflammation. Syndesmophytes, however, may not always be visible by MRI because they may be difficult to distinguish from fibrous tissue unless there is concomitant active inflammation or fatty deposition (Figs. 11, 16) [15, 20].
The possibility of visualizing disease activity by MRI has increased its use to monitor AS, especially during anti-TNF (
Other Forms of SpA
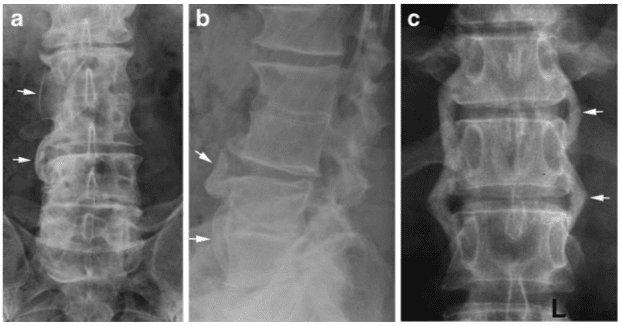
Radiographic changes in reactive and psoriatic arthritis are often characterized by voluminous non-marginal syndesmophytes (
Reactive arthritis is self-limiting in most patients. However, in patients with chronic reactive arthritis and HLA
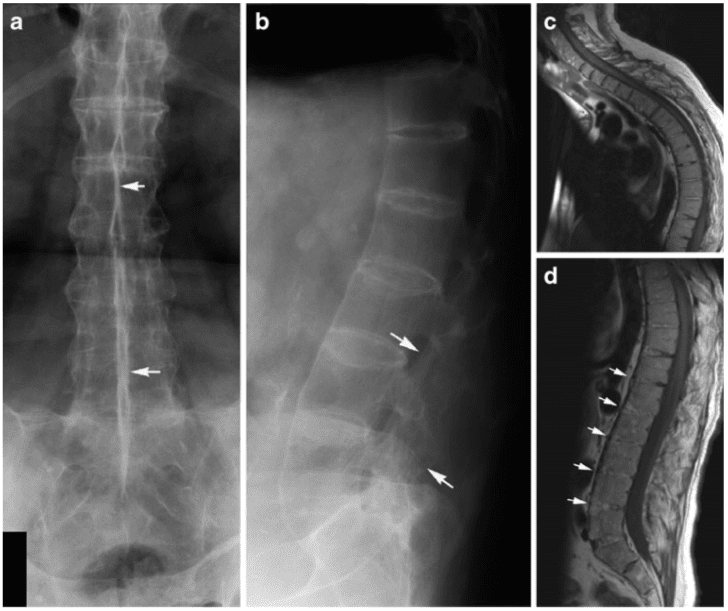
in a 55-year-old man showing vertebral fusion due to syndesmophytes crossing the intervertebral spaces in addition to fusion of the apophyseal joints (bamboo spine). The interspinous ligaments are ossified, presenting as a slim ossified streak on the frontal radiograph (dagger sign; arrows). MRI, sagittal T1- weighted images of (c) the cervico-thoracic and (d) lumbar region, respectively, shows a general narrowing of the intervertebral discs with partial osseous fusion of the vertebral bodies, especially in the lumbar region (arrows). In addition a characteristic AS deformity with reduced lumbar lordosis and thoracic kyphosis.
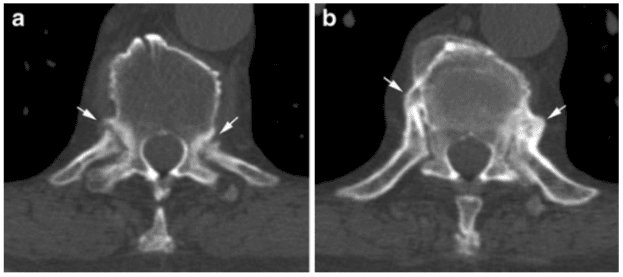
Axial psoriatic arthritis (PsA) occurs in approximately 50% of patients with peripheral PsA [31]. It differs radiographically from AS by the voluminous paravertebral ossifications and the occurrence of spinal changes without concomitant sacroiliitis in 10% of patients [32]. Axial
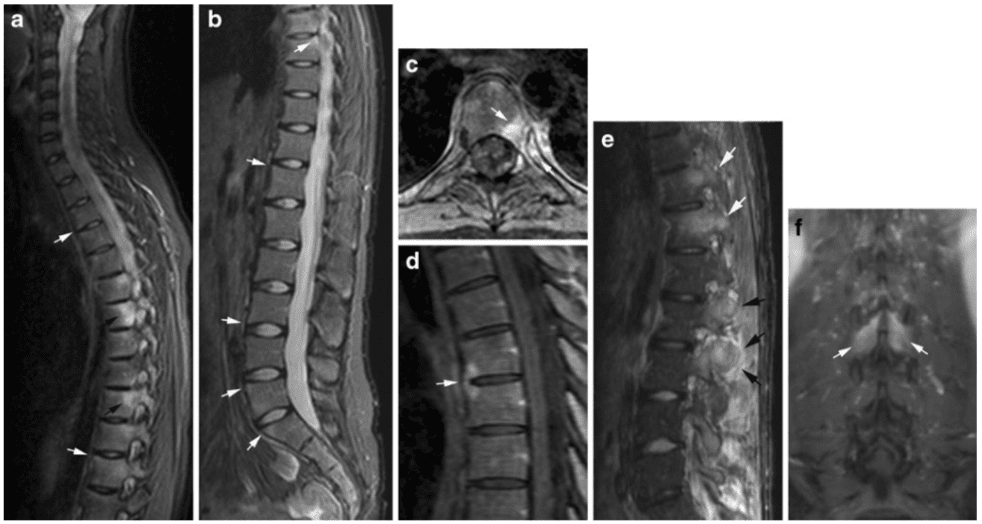
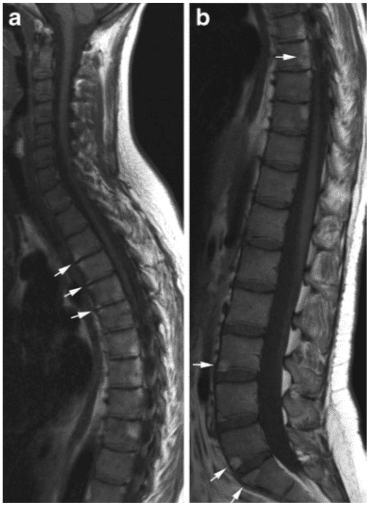
Chronic changes in AS by MRI. Sagittal T1 (a) the cervico-thoracic and (b) the lumbar spine of the patients shown in Fig. 10. There are multiple fatty marrow depositions at vertebral corners and also posteriorly in thoracic vertebral bodies (b, arrows). This was observed to have developed since the MRI performed 3 years previously (shown in Fig. 16 a-d) and corresponds to areas of previous inflammation.
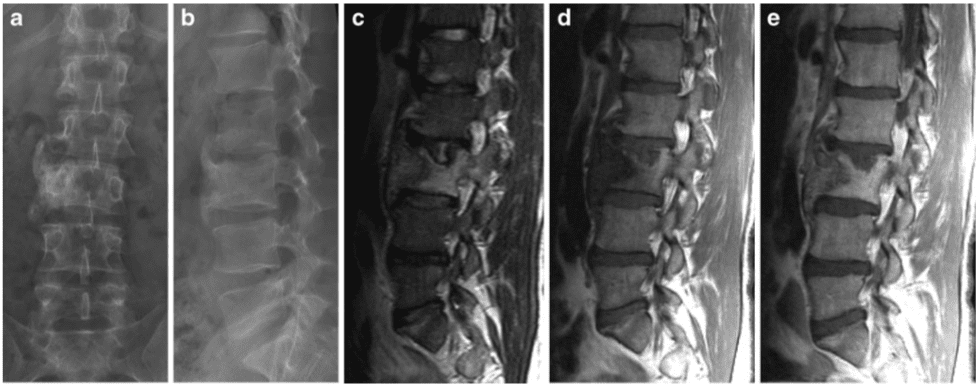
In patients with enteropathic arthritis associated with Crohn’s disease or ulcerative colitis, the spine is often osteoporotic with various accompanying SpA features by radiography, mostly AS-like changes. However, by MRI there may be more pronounced inflammation in the posterior ligaments than seen in the other forms of SpA (Fig. 21).
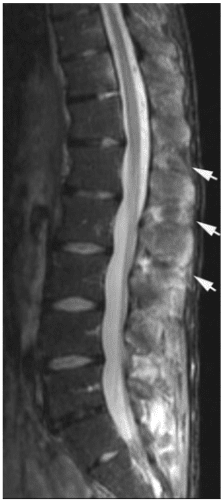

Rheumatoid arthritis of the spine can cause neck pain, back pain, and/or radiating pain in the upper and lower extremities. In severe cases, RA can also lead to the degeneration of the spine, resulting in the compression or impingement of the spinal cord and/or the spinal nerve roots. As a chiropractor, we offer diagnostic imaging to help determine a patient’s health issue, in order to develop the best treatment program.
Dr. Alex Jimenez D.C., C.C.S.T.
Conclusion
Radiography is still valuable in the diagnosis of spinal inflammatory disorders. It is necessary for visualizing instability and is superior to MRI for detecting syndesmophytes. However, MRI and CT can detect signs of spinal involvement before they can be visualized by radiography. MRI adds information about
Computed tomography is particularly valuable in the detection of fracture and minor osseous lesions as well as in the evaluation of pseudo-arthrosis. In conclusion, rheumatoid arthritis most commonly affects the structure and function of your hands, wrists, elbows, hips, knees, ankles and feet, however, people with this chronic inflammatory disease can experience back pain. Imaging the spine in arthritis is fundamental to determine treatment. The scope of our information is limited to chiropractic as well as to spinal injuries and conditions. To discuss the subject matter, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .
Curated by Dr. Alex Jimenez
1. Paus AC, Steen H, Roislien J, Mowinckel P, Teigland J (2008) High mortality rate in rheumatoid arthritis with subluxation of the cervical spine: a cohort study of operated and nonoperated patients. Spine 33(21):2278–2283
2. Kim DH, Hilibrand AS (2005) Rheumatoid arthritis in the cervical spine. J Am Acad Orthop Surg 13(7):463–474
3. Younes M, Belghali S, Kriaa S, Zrour S, Bejia I, Touzi M et al (2009) Compared imaging of the rheumatoid cervical spine: prevalence study and associated factors. Joint Bone Spine 76 (4):361–368
4. Riew KD, Hilibrand AS, Palumbo MA, Sethi N, Bohlman HH (2001) Diagnosing basilar invagination in the rheumatoid patient. The reliability of radiographic criteria. J Bone Joint Surg Am 83 (2):194–200
5. Ishii K, Matsumoto M, Takahashi Y, Okada E, Watanabe K, Tsuji T et al (2010) Risk factors for development of subaxial subluxations following atlantoaxial arthrodesis for atlantoaxial subluxations in rheumatoid arthritis. Spine 35(16):1551–1555
6. Iizuka H, Sorimachi Y, Ara T, Nishinome M, Nakajima T, Iizuka Y et al (2008) Relationship between the morphology of the atlanto-occipital joint and the radiographic results in patients with atlanto-axial subluxation due to rheumatoid arthritis. Eur Spine J 17(6):826–830
7. Narvaez JA, Narvaez J, Serrallonga M, De Lama E, de AM, Mast R et al (2008) Cervical spine involvement in rheumatoid arthritis:
correlation between neurological manifestations and magnetic resonance imaging findings. Rheumatology (Oxford) 47 (12):1814–1819
8. Dougados M, van der Linden S, Juhlin R, Huitfeldt B, Amor B, Calin A et al (1991) The European Spondylarthropathy Study Group preliminary criteria for the classification of spondylarthr- opathy. Arthritis Rheum 34:1218–1227
9. Rudwaleit M, van der Heijde D, Landewe R, Listing J, Akkoc N, Brandt J et al (2009) The Development of Assessment of SpondyloArthritis international Society (ASAS) classification criteria for axial spondyloarthritis (Part II): validation and final selection. Ann Rheum Dis 68(6):777–783
10. Sieper J, Rudwaleit M, Khan MA, Braun J (2006) Concepts and epidemiology of spondyloarthritis. Best Pract Res Clin Rheumatol 20(3):401–417
11. van der Linden S, Valkenburg HA, Cats A (1984) Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria. Arthritis Rheum 27:361– 268
12. Maksymowych WP, Chiowchanwisawakit P, Clare T, Pedersen SJ, Ostergaard M, Lambert RG (2009) Inflammatory lesions of the spine on magnetic resonance imaging predict the development of new syndesmophytes in ankylosing spondylitis: evidence of a relationship between inflammation and new bone formation. Arthritis Rheum 60(1):93–102
13. Sieper J, Rudwaleit M, Baraliakos X, Brandt J, Braun J, Burgos- Vargas R et al (2009) The Assessment of SpondyloArthritis international Society (ASAS) handbook: a guide to assess spondyloarthritis. Ann Rheum Dis 68(Suppl 2:ii):1–44
14. Park WM, Spencer DG, McCall IW, Ward J, Buchanan WW, Stephens WH (1981) The detection of spinal pseudarthrosis in ankylosing spondylitis. Br J Radiol 54(642):467–472
15. Madsen KB, Jurik AG (2009) MRI grading method for active and chronic spinal changes in spondyloarthritis. Clin Radiol 65:6–14
16. Feldtkeller E, Vosse D, Geusens P, van der Linden S (2006) Prevalence and annual incidence of vertebral fractures in patients with ankylosing spondylitis. Rheumatol Int 26(3):234–239
17. Thomsen AH, Uhreholt L, Jurik AG, Vesterby A (2010) Traumatic death in ankylosing spondylitis—a case report. J Forensic Sci 55(4):1126–1129
18. Bennett AN, Rehman A, Hensor EM, Marzo-Ortega H, Emery P, McGonagle D (2009) Evaluation of the diagnostic utility of spinal magnetic resonance imaging in axial spondylarthritis. Arthritis Rheum 60(5):1331–1341
19. Appel H, Loddenkemper C, Grozdanovic Z, Ebhardt H, Dreimann M, Hempfing A et al (2006) Correlation of histopathological findings and magnetic resonance imaging in the spine of patients with ankylosing spondylitis. Arthritis Res Ther 8(5):R143
20. Braun J, Baraliakos X, Golder W, Hermann KG, Listing J, Brandt J et al (2004) Analysing chronic spinal changes in ankylosing spondylitis: a systematic comparison of conventional x rays with magnetic resonance imaging using established and new scoring systems. Ann Rheum Dis 63(9):1046–1055
21. Baraliakos X, Listing J, Brandt J, Haibel H, Rudwaleit M, Sieper J et al (2007) Radiographic progression in patients with ankylosing spondylitis after 4 years of treatment with the anti- TNF-alpha antibody infliximab. Rheumatology (Oxford) 46 (9):1450–1453
22. Lambert RG, Salonen D, Rahman P, Inman RD, Wong RL, Einstein SG et al (2007) Adalimumab significantly reduces both spinal and sacroiliac joint inflammation in patients with ankylos- ing spondylitis: a multicenter, randomized, double-blind, placebo- controlled study. Arthritis Rheum 56(12):4005–4014
23. Baraliakos X, Landewe R, Hermann KG, Listing J, Golder W, Brandt J et al (2005) Inflammation in ankylosing spondylitis: a systematic description of the extent and frequency of acute spinal changes using magnetic resonance imaging. Ann Rheum Dis 64
(5):730–734
24. Khanna M, Keightley A (2005) MRI of the axial skeleton
manifestations of ankylosing spondylitis. Clin Radiol 60(1):135–136
25. Levine DS, Forbat SM, Saifuddin A (2004) MRI of the axial skeletal manifestations of ankylosing spondylitis. Clin Radiol 59
(5):400–413
26. Baraliakos X, Hermann KG, Landewe R, Listing J, Golder W,
Brandt J et al (2005) Assessment of acute spinal inflammation in patients with ankylosing spondylitis by magnetic resonance imaging: a comparison between contrast enhanced T1 and short tau inversion recovery (STIR) sequences. Ann Rheum Dis 64 (8):1141–1144
27. Gaspersic N, Sersa I, Jevtic V, Tomsic M, Praprotnik S (2008) Monitoring ankylosing spondylitis therapy by dynamic contrast- enhanced and diffusion-weighted magnetic resonance imaging. Skeletal Radiol 37(2):123–131
28. Weber U, Maksymowych WP, Jurik AG, Pfirrmann CW, Rufibach K, Kissling RO et al (2009) Validation of whole-body against conventional magnetic resonance imaging for scoring acute inflammatory lesions in the sacroiliac joints of patients with spondylarthritis. Arthritis Rheum 61(7):893–899
29. Weber U, Hodler J, Jurik AG, Pfirrmann CW, Rufibach K, Kissling RO et al (2010) Assessment of active spinal inflamma- tory changes in patients with axial spondyloarthritis: validation of whole body MRI against conventional MRI. Ann Rheum Dis 69 (4):648–653
30. Helliwell PS, Hickling P, Wright V (1998) Do the radiological changes of classic ankylosing spondylitis differ from the changes found in the spondylitis associated with inflammatory bowel disease, psoriasis, and reactive arthritis? Ann Rheum Dis 57(3):135–140
31. Chandran V, Barrett J, Schentag CT, Farewell VT, Gladman DD (2009) Axial psoriatic arthritis: update on a longterm prospective study. J Rheumatol 36(12):2744–2750
32. Lubrano E, Marchesoni A, Olivieri I, D’Angelo S, Spadaro A, Parsons WJ et al (2009) Psoriatic arthritis spondylitis radiology index: a modified index for radiologic assessment of axial involvement in psoriatic arthritis. J Rheumatol 36(5):1006–1011
33. Hanly JG, Russell ML, Gladman DD (1988) Psoriatic spondy- loarthropathy: a long term prospective study. Ann Rheum Dis 47 (5):386–393
34. Takigawa T, Tanaka M, Nakanishi K, Misawa H, Sugimoto Y, Takahata T et al (2008) SAPHO syndrome associated spondylitis. Eur Spine J 17(10):1391–1397

Additional Topics: Acute Back Pain
Back pain is one of the most prevalent causes of disability and missed days at work worldwide. Back pain attributes to the second most common reason for doctor office visits, outnumbered only by upper-respiratory infections. Approximately 80 percent of the population will experience back pain at least once throughout their life. The spine is a complex structure made up of bones, joints, ligaments, and muscles, among other soft tissues. Because of this, injuries and/or aggravated conditions, such as herniated discs, can eventually lead to symptoms of back pain. Sports injuries or automobile accident injuries are often the most frequent cause of back pain, however, sometimes the simplest of movements can have painful results. Fortunately, alternative treatment options, such as chiropractic care, can help ease back pain through the use of spinal adjustments and manual manipulations, ultimately improving pain relief.

EXTRA IMPORTANT TOPIC: Sciatica Pain Chiropractic Therapy
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card