How does pain become chronic? Pain can be a complex condition, as it involves both physiological and psychological components. When an individual experiences an injury, the damaged tissues trigger and send pain signals to the brain. This is how the body alerts that there is something wrong, and thus prevents further damage. Those pain signals travel to the brain, stimulate the nerves, and cause a sensation known as pain.
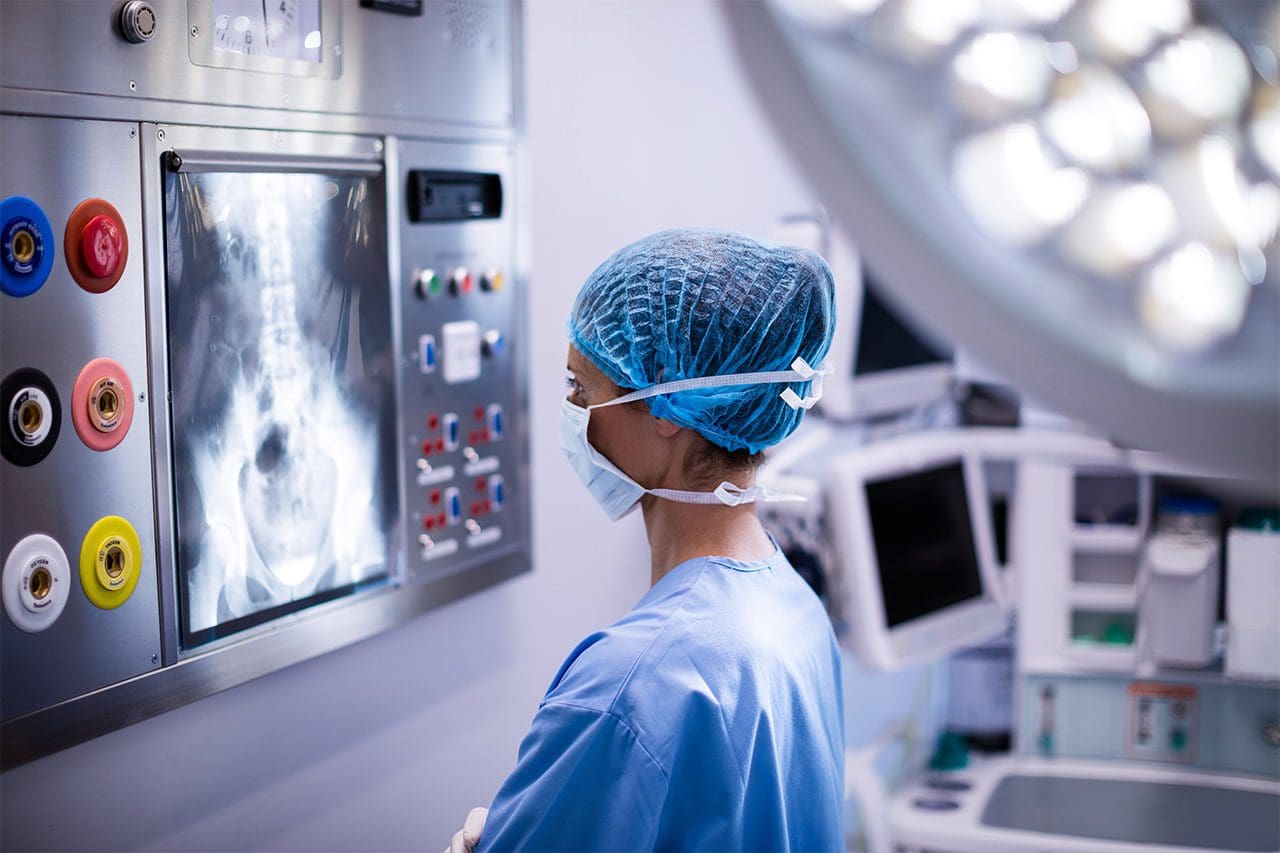
Table of Contents
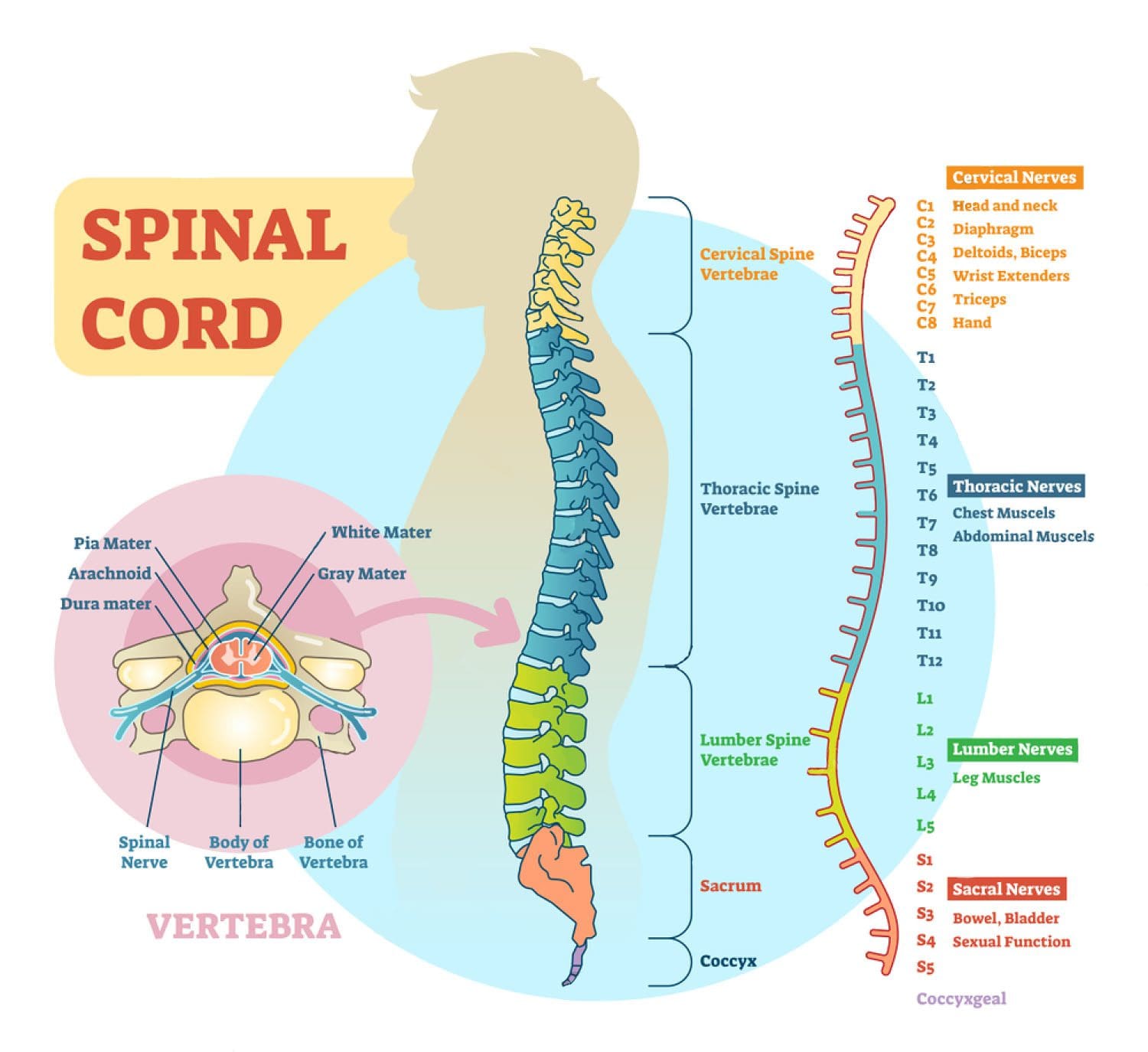
Nerves and the brain
Nerves control the body’s functions like the organs, sensation, and movement. The nervous system receives information and generates the correct response. Two major types of nerves are sensory and motor. Sensory nerves relay information like touch, temperature, and pain to the brain and spinal cord. Motor nerves relay signals from the brain back to the muscles, which causes them to contract voluntarily or reflexively.
The peripheral nervous system is the combined millions of nerves throughout the body. The peripheral nervous system’s nerves relay signals/messages to the central nervous system, which is comprised of the brain and spinal cord.
When pain becomes chronic the brain fails to process these signals correctly and the individual continues to feel pain after the injury has healed or improved. As time goes on the nerves that send the pain signals are more methodical in their signaling. This means more signals than normally will be sent and are far more intense. Conditions like cancer and diabetes can cause tissue and nerve damage throughout the body.
Acute vs. Chronic
Acute pain has a short duration of around three months or less. The causes are usually clear and not as difficult to diagnose. The underlying factor/s like an injury is resolved the pain also goes away. As the pain is gone, the individual no longer has problems carrying out daily activities. A few causes of acute pain are:
- Surgical procedures
- Dental procedures
- Bone fractures
- Burns
- Open wounds
- Childbirth
Chronic pain is defined as pain that lasts three to six months with some conditions going for years. Individuals can experience chronic pain weeks and months possibly years after the injury took place. And it can happen without any apparent cause. Many cases often involve more than one factor. This causes significant problems with daily activities. When pain becomes chronic it is often associated with conditions like cancer, diabetes, and arthritis.
CP and CPS
Chronic pain is defined as any type of pain that persists for six months or longer. Chronic pain syndrome is a collection of conditions that are associated with chronic pain. These conditions can make the pain worse or cause other complications like sleep problems, anger, anxiety, and depression.

Causes
Doctors don’t know exactly what causes chronic pain syndrome. It often starts with an injury or painful condition such as:
- Arthritis
- Broken bones
- Back pain
- Cancer
- Headaches
- Joint problems
- Muscle strains and sprains
- Repetitive strain injuries
- Fibromyalgia
- Nerve injury/damage
- Lyme disease
- Ulcers
- Inflammatory bowel disease
- Irritable bowel syndrome
- Surgery
Diagnosis
A doctor will go over an individual’s medical history, illnesses, or injuries that could have started the pain. They will ask questions to learn more about the type of pain being felt and how long. Questions can include:
- When did the pain begin?
- Where on the body does it hurt?
- What does the pain feel like – Throbbing, Pounding, Shooting, Sharp, Pinching, Stinging, Burning
- The severity of the pain on a scale of 1 to 10
- What sets the pain off?
- What makes it worse?
- Have any treatments helped?
Imaging tests can show if there is joint damage or other problems:
- Computed tomography is a powerful X-ray that generates detailed images.
- Magnetic resonance imaging uses magnets and radio waves to take pictures of the organs and structures.
- X-rays use radiation in very low doses to create images of the body’s structures.
Talk with a chiropractor to understand how a customized treatment plan for chronic pain is developed.
Chronic Pain Chiropractor
Dr. Alex Jimenez’s Blog Post Disclaimer
The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.*
Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation as to how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas& New Mexico*
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card


