Table of Contents
Introduction
The body has many nerves that intertwine and branch out from the spinal cord in the central nervous system. These nerves provide many functions that the body needs to work correctly, from motor function on the arms, legs, and neck to sensory functions like perceiving how much light comes into the eyes, that sense of fullness in the gut system, and when something is touching the skin. The body needs these nerves for everyday function and when a person feels pain from accidents and injuries. When there are factors that cause nerve damage or even gut issues that are internally affecting the body, it can cause many symptoms and cause a person to feel gloomy. Today’s article looks at the parasympathetic nervous system, how it affects the gut microbiota, and how autonomic neuropathy disrupts the gut system in many individuals. Refer patients to certified, skilled providers specializing in gut treatments for individuals that suffer from autonomic neuropathy. We guide our patients by referring to our associated medical providers based on their examination when it’s appropriate. We find that education is critical for asking insightful questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, it may. If you are uncertain, here is the link to all the insurance providers we cover. If you have any questions or concerns, please call Dr. Jimenez at 915-850-0900.
What Is The Parasympathetic Nervous System?
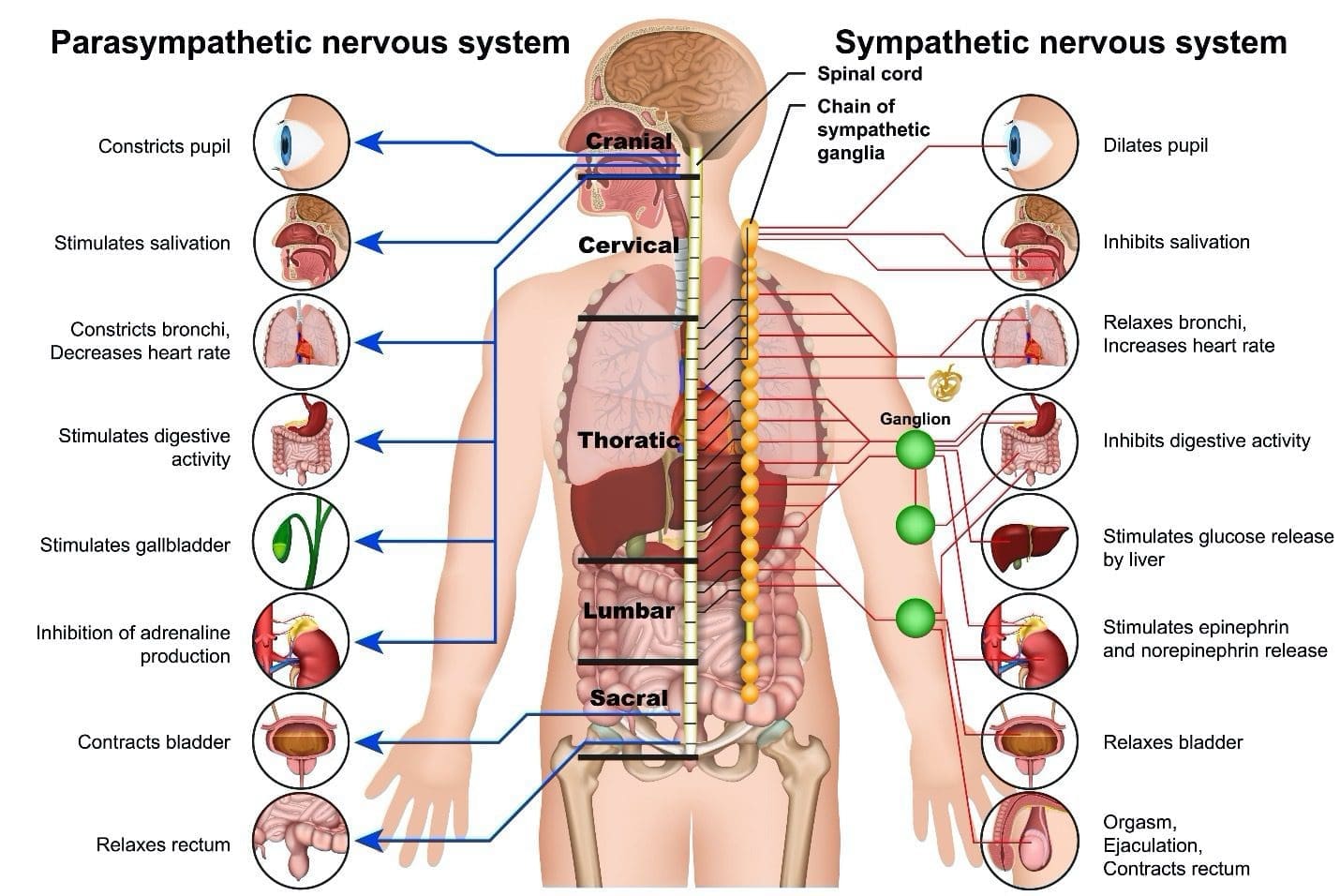
Have you experienced gut issues affecting your body? How about feeling dizzy or faint when standing up? Does it seem difficult to adjust your eyesight from dark to light? Or have you experienced gut inflammation? These signs and symptoms are usually affected when the parasympathetic nerves are damaged and causing gut issues in the body. The parasympathetic nervous system. as research has defined it, conserves the body’s energy to be used for a later date while regulating bodily functions. These nerves help the body go into a “resting” condition that allows the body to work in a less stressful environment than the sympathetic nervous system, which drives the “fight or flight” response. The parasympathetic nerves also help with the GI tract, as additional research shows the parasympathetic nervous system helps exert excitatory and inhibitory GI control and motility in the intestines. The parasympathetic nerves and the gut microbiota are connected as they help influence the body’s homeostasis.
How Does It Affect The Gut Microbiota?
So the brain and the gut are connected to the body as they help send the information back and forth to provide the body’s homeostasis and immune function in preventing diseases. So for the parasympathetic nervous system and how it affects the gut microbiota, it’s all due to the vagus nerve that keeps the gut microbiota functioning and doing its job to support the body. Research studies have shown that the vagus nerve is the primary component of the parasympathetic nervous system. The vagus nerve helps with the bi-directional communication between the brain and the gut system by overseeing the crucial bodily functions. Some of the tasks that the parasympathetic nervous system does for the gut microbiota include:
- Mood control
- Immune response
- Heart rate
- Digestion
- Influences gastrointestinal homeostasis regulation
- Connect emotional and cognitive areas of the brain
An Overview On The Parasympathetic Nerves-Video
Feeling inflammatory effects inside your gut? How about feeling dizzy by just standing for a little bit? Do you have difficulty eating or have a loss of appetite? Many of these signs of parasympathetic nerves are affected, causing abnormalities in the gut microbiota. The video above explains what the parasympathetic nervous system does and how it plays its role in the entire body. The parasympathetic nervous system also has a partnership with the gut microbiota. Research studies mentioned that the interaction between the parasympathetic nervous system and the gut microbiome ensures the proper maintenance of homeostasis and cognitive functions for the body. The gut-brain axis helps promote optimal bodily function while ensuring that the motor-sensory parts are doing their jobs.
How Autonomic Neuropathy Affects The Gut System
Injuries affecting the gut microbiota and the parasympathetic nervous system can cause gut inflammation in the intestines and nerve damage to the nervous system. This is known as autonomic neuropathy, and research shows that this type of neuropathy causes body and gut issues like diabetes and gastrointestinal motility and contributes to other GI symptoms. Other research studies have found that autonomic neuropathy can alter the gut microbiota’s homeostasis regulation. When this happens, the body will start to have various symptoms affecting each organ and making them dysfunctional. The body will develop more symptoms when the gut microbiota becomes affected. These symptoms cause a decrease in vagal outflow or an increase in sympathetic activity, which will be associated with a slow decreased gastrointestinal motility.
Conclusion
The gut and nervous systems have a bi-directional communication that helps provide the body with proper immune support and metabolizing homeostasis for functionality. The nerves in the nervous system are branched out from the spinal cord and help offer many functions to the arms, organs, legs, and muscle tissues. The parasympathetic nerves in the nervous system help the body rest and digest the nutrients provided to the body. When the nerves or the gut suffer from damage, it can cause various problems that cause dysfunction to the motor-sensory functions of the body. When this happens, many individuals can find different treatments to restore body functions to the gut and the parasympathetic nerves and reduce the symptoms that come with it.
References
Breit, Sigrid, et al. “Vagus Nerve as Modulator of the Brain-Gut Axis in Psychiatric and Inflammatory Disorders.” Frontiers in Psychiatry, Frontiers Media S.A., 13 Mar. 2018, www.ncbi.nlm.nih.gov/pmc/articles/PMC5859128/.
Browning, Kirsteen N, and R Alberto Travagli. “Central Nervous System Control of Gastrointestinal Motility and Secretion and Modulation of Gastrointestinal Functions.” Comprehensive Physiology, U.S. National Library of Medicine, Oct. 2014, www.ncbi.nlm.nih.gov/pmc/articles/PMC4858318/.
Kornum, Ditte S, et al. “Assessment of Gastrointestinal Autonomic Dysfunction: Present and Future Perspectives.” Journal of Clinical Medicine, MDPI, 31 Mar. 2021, www.ncbi.nlm.nih.gov/pmc/articles/PMC8037288/.
Mayer, Emeran A. “Gut Feelings: The Emerging Biology of Gut-Brain Communication.” Nature Reviews. Neuroscience, U.S. National Library of Medicine, 13 July 2011, www.ncbi.nlm.nih.gov/pmc/articles/PMC3845678/.
Tindle, Jacob, and Prasanna Tadi. “Neuroanatomy, Parasympathetic Nervous System – Statpearls – NCBI Bookshelf.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 5 Nov. 2021, www.ncbi.nlm.nih.gov/books/NBK553141/.
Tougas, G. “The Autonomic Nervous System in Functional Bowel Disorders.” Canadian Journal of Gastroenterology = Journal Canadien De Gastroenterologie, U.S. National Library of Medicine, Mar. 1999, pubmed.ncbi.nlm.nih.gov/10202203/.
Disclaimer
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card