Chronic Pain: Pain That Doesn’t Stop or Go Away
Chronic pain is pain that is ongoing and does not stop for six months. Even when the injuries or illness/condition that caused the pain are healed or go away, the pain stays. This can go on for weeks, months, and even years. Acute pain comes on rapidly and can be traced to a direct cause. Chronic pain can linger and can be quite a challenge in diagnosing the root cause. This is a situation for many individuals, as there is pain present, but they can’t figure out where it is coming from.
Chronic pain is considered a disease or condition. Normally pain is a symptom that is presenting as a warning that something is wrong with the body. When the pain becomes chronic, it is no longer a warning of something wrong with the body. It is an ailment.

Another definition is pain that’s present even without a visible injury or disease that is causing it. Chronic pain can be difficult to define accurately because it can take on so many forms. Therefore, determining the type of pain is the objective toward finding a treatment that will help deal with whatever form of chronic pain it is.
Table of Contents
Chronic Pain Types
Chronic pain is placed into two categories.
These categories help physicians develop individually customized treatments because everyone and their pain type is unique and needs to be approached and treated uniquely. General forms of chronic pain are:
Neuropathic pain
This is pain caused by damage to or malfunction of the nerves.
Nociceptive pain
Nociceptors are receptors in the nervous system that are activated when an injury occurs. If there is no injury from outside of the nervous system, the nociceptors do not get activated. Therefore, nociceptive pain is caused by an injury to an area of the body that is not the nerves. The nociceptors are still sending/relaying pain messages with chronic pain after the injury that created the pain has healed.
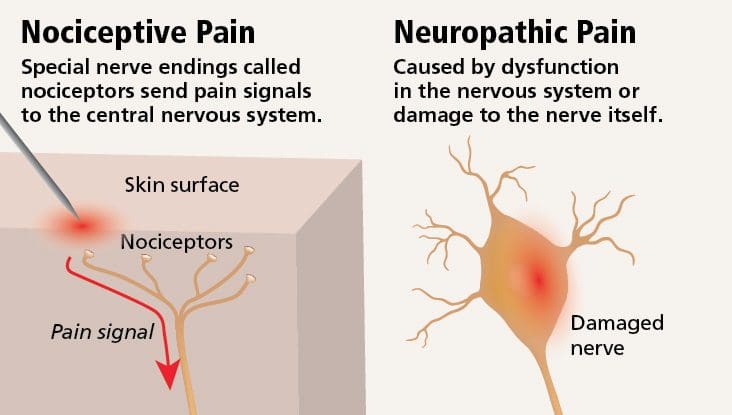
Neuropathic Pain
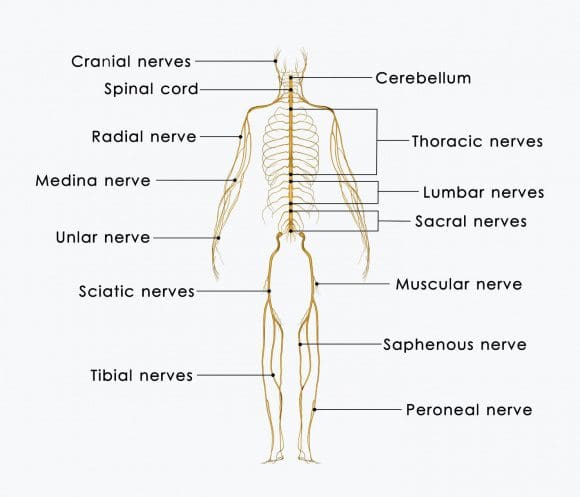
The peripheral nervous system includes all the nerves going to and from the spinal cord. These nerves send pain signals to the brain. If they get injured, neuropathic pain can develop. This is pain caused by injury to these nerves. The term peripheral neuropathy is another way of saying neuropathic pain. This comes from damage to the peripheral nervous system. Central nervous system injury/damage can also trigger neuropathic pain. Chronic neuropathic pain can be extremely challenging to treat because of the difficulty of finding where and how the nerves are damaged/injured.
Nociceptive Pain
An injury or disease causes nociceptive pain to an area of the body. It’s an injury or disease that stimulates the nociceptors. There are various types of chronic nociceptive pain:
Somatic pain
Somatic pain comes from an injury/s that happen to the outer body like the:
- Skin
- Muscles
- Ligaments
- Tendons
- Joints
- Bones
Somatic pain can usually be easier to diagnose as the pain can be sharp or throbbing depending on what part of the body is injured. Bone pain is somatic pain, as the bones can ache. If the bones are weakened from other condition/s like cancer or osteoporosis, there can be a very achy and intense dull pain. Bone pain can also be acute. For example, a bone break is an acute pain. When the bone heals, but there is still throbbing pain that could be constant or comes and goes could be considered chronic bone pain.
Muscle pain is also considered a form of somatic pain. However, chronic muscle pain is more than a strain. The muscles can go through chronic muscle spasms that cause them to become tense. Muscle overload can cause intense/constant pain throughout the body, especially in the back. Muscle pain can also develop from chronic conditions, like fibromyalgia.
Visceral pain
The viscera are the internal organs, specifically those in the abdomen and chest cavity. The stomach is a perfect example of a visceral organ. Not all organs have nociceptors, so they cannot send pain signals if they are injured. In this type, a dull ache will be felt but could be difficult to pinpoint. Visceral pain can also present referred pain. This means that the brain has difficulty calculating if the pain is coming from an organ or another part of the body. An example is a kidney problem where the low back is in pain.
Figuring out what type of chronic pain is presenting can be a difficult process. As there are many types and trying to diagnose without any noticeable injury or disease is a challenge. Pain is a subjective experience that must be described in detail by a doctor or specialist as long as the individual works together with a doctor. Then the best treatment option can be generated.

Symptoms
It can take on many forms like:
- Aches/Aching
- Burning sensation of pain
- An electric sensation of pain
- Sharp pain
- Shooting pain
- Soreness
- Stiffness
- Throbbing pain
- Tightness
Chronic pain definitely leads to other issues, specifically social and emotional like:
- Sleeplessness
- Energy is drained
- Depression
- Withdraw from family friends activities normally enjoyed
- The immune system becomes weakened from a tremendous amount of body energy dealing with the pain

Proper Diagnosis
Obtaining a proper diagnosis of the cause of chronic pain is essential to creating the most optimal treatment plan. The severity and cause of chronic pain may require an individual to see various specialists in addition to the primary caregiver. These could be a:
- Chiropractor
- Physical therapist
- Pain medicine specialist
- Orthopedic spine surgeon
- Neurosurgeon
- Physiatrist
- Rheumatologist
As time goes on, chronic pain can change and need reevaluation that could affect how it is treated and managed.

Treatment
Treatment and therapy options that could be offered are:
Chiropractic
Depending on the diagnosis, a doctor could recommend chiropractic medicine. Two weeks of regular manipulation can significantly improve individuals with chronic low back pain with referred leg pain.
Physical Therapy
Stretching and strengthening the muscles are vital in the treatment of chronic pain. A physical therapist could include:
- Ice
- Heat
- Transcutaneous electrical nerve stimulation (TENS)
- Ultrasound
- Myofascial release
- Stretching exercises
- Strengthening exercises
Meds
Different meds could be prescribed to treat pain, inflammation, muscle spasms, and neuropathic pain. This could be combined with meds that treat accompanying symptoms/conditions like sleep problems, depression, and anxiety.
Surgery
A doctor could recommend spinal injections, spinal cord stimulation, drug pump, or spinal surgery. If there is uncertainty about the recommended treatment plan, then get a second opinion.
Skills for coping
Mood and psychological perspective can affect the level of pain. A trained specialist could educate and train an individual with relaxation and coping skills.
Complementary care
Doctors are now recommending several complementary therapies like acupuncture and other forms of traditional Chinese medicine. Ask a doctor about this option. It is often used in conjunction with conventional and alternative medicine/therapy/treatment programs.
Chiropractic Management
A chiropractor will do a physical exam and specific tests to help them diagnose the root cause of the pain. Once diagnosed, the chiropractor will develop a customized treatment plan. The treatment could include spinal manipulation, manual therapies, and therapeutic exercises.
A chiropractor will work with the individual in developing an optimal treatment plan geared to that individual’s needs. Once the pain is completely addressed, the individual will gradually and progressively increase daily activities.
Chiropractic Chronic Pain Treatment
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card

