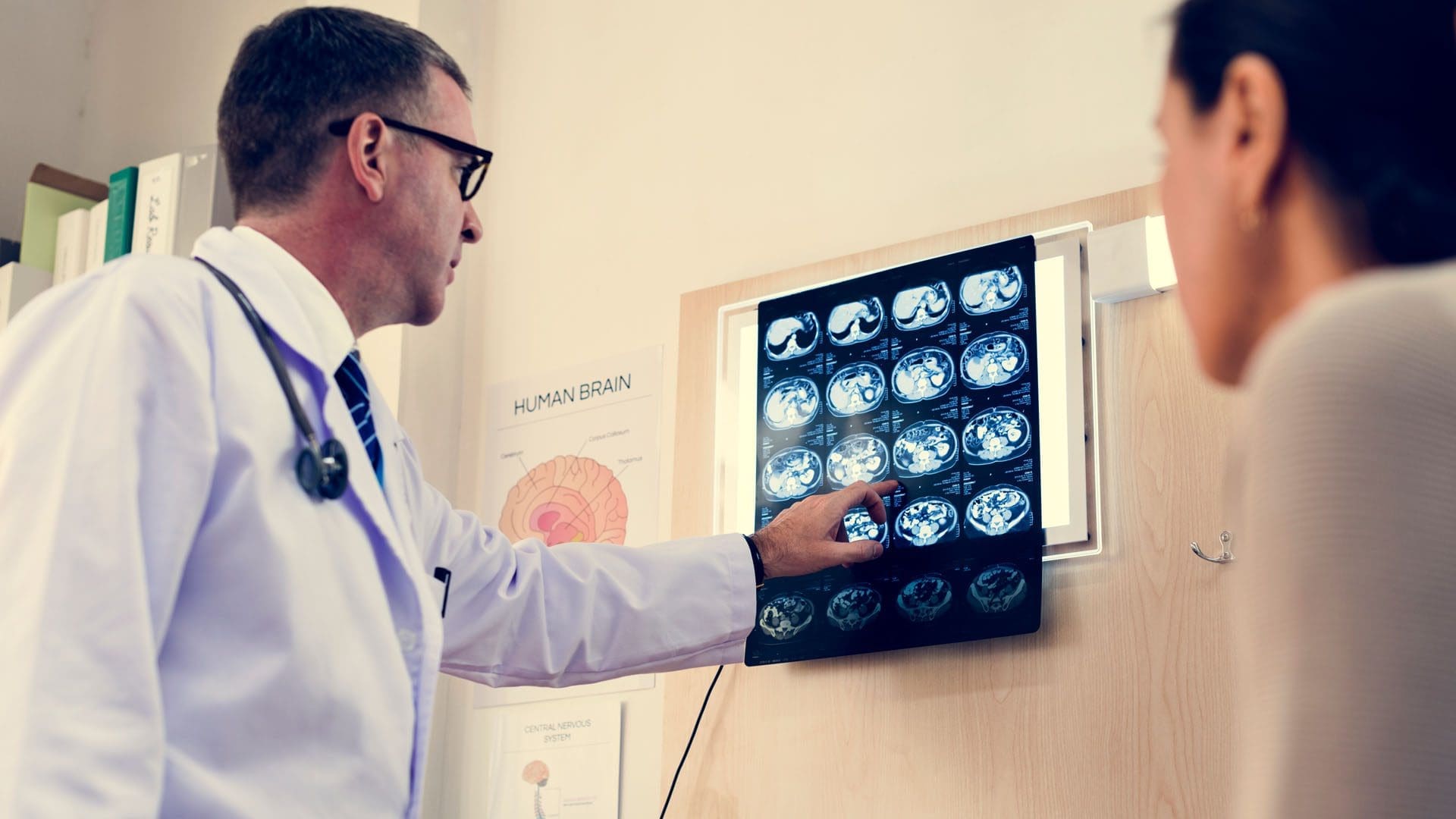
Every year an estimated 3.8 million people in the United States sustain mild traumatic brain injuries (MTBI) or concussions. Many of these injuries are due to sports-related activities, work related injuries, motor vehicle accidents, and military operations. It is also estimated that as many as 50% of MTBIs are never reported because the patient does not seek medical attention. This makes it difficult to get a solid number on how many there actually are, but it is a prevalent condition.
Table of Contents
The Brain and Skull
A patient does not have to actually hit their head to sustain an MTBI. It can be caused by whiplash even though the person never hit their head. The reason for this lies in the construction of the brain and skull.
The brain is very soft, some experts compare the texture to that of soft butter. The skull is designed to protect the brain, and it is extremely hard. If you run your hand over your head, you may feel some lumps and bumps, it may not feel completely even, but the surface will be smooth.
The same cannot be said for the inside of the skull. There are a number of boney ridges on the inside that are quite sharp. The design is intended to keep the brain in place.
When the head is hit or is jolted hard enough it caused the brain to shift inside of the skull, coming into contact with those boney ridges – sometimes forcefully. This can cause damage and the result in a brain injury. The harder the jolt, the more serious the injury may be.
Symptoms of Mild Traumatic Brain Injury
Part of the problem with MTBI is that the symptoms may not show up immediately. They could emerge weeks or even months after the incident making it unlikely that the symptoms will be tracked back and connected to it.
Common symptoms of MTBI include:
- Nausea
- Confusion
- Moodiness
- Photophobia
- Problems with balance
- Difficulty focusing or concentrating
- Anger issues, outbursts
- Sleep issues
- Problems with memory
- Social isolation
- Fatigue – mental or physical
- Elevated anxiety
- Vision problems
- Sound sensitivity
Often, MTBI is called a “silent epidemic” because the symptoms that it causes are usually not visible and may not be immediately connected to the injury. Depression, anxiety, angry outbursts, and impaired memory are more likely to be considered a psychiatric issue instead of a neurological one. The symptoms can be debilitating just the same.
Evaluation and diagnosis of an MTBI
Chiropractors routinely treat patients with Mild Traumatic Brain Injuries. When they are presented with a patient that they know has sustained a head injury, or if they suspect a brain injury based on specific symptoms, they use the Sports Concussion Assessment Tool 2 (SCAT2) to determine the severity. The SCAT2 helps the chiropractor create evaluate the physical signs, symptoms, sideline assessment using Maddocks score, Glasgow Coma Scale, coordination, balance, and cognitive.
As they evaluate the patient, they look for specific markers that indicate the patient is experiencing worsening neurological symptoms. These include:
- Loss of consciousness
- Vomiting
- Headaches get worse
- Increased confusion
- Weakness on one side or in one leg or arm
- Blurred vision
- Dilated pupils
- Balance or coordination problems
Chiropractic Treatment for MTBI
A head injury usually involves a neck injury as well. The chiropractor may use a variety of techniques to treat the patient, including spinal manipulation, massage, and bracing. The patient will also be advised to avoid anti-inflammatory medication, aspirin, alcohol, and sleep aids, using acetaminophen for pain as needed. If the patient needs to see another doctor or specialist, the chiropractor will refer them.
Chiropractic Migraine Treatment
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card