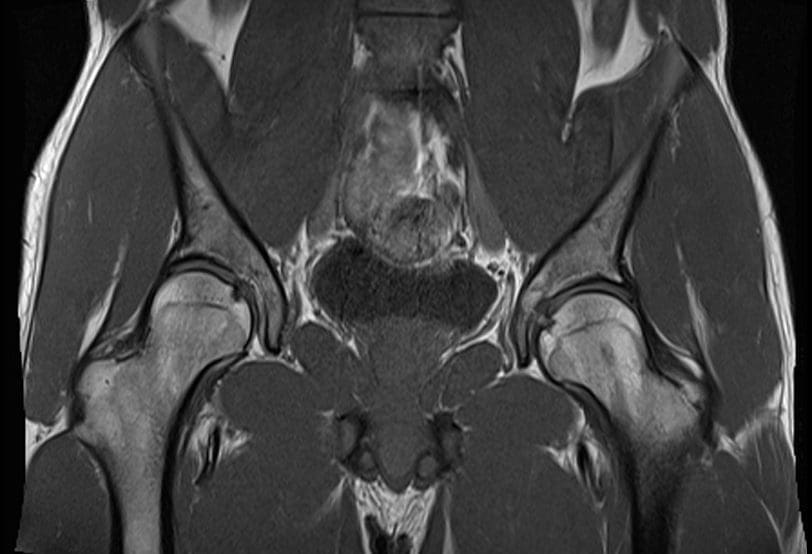
Athletic pubalgia, also known as a hockey hernia, hockey groin, Gilmore’s Groin, sports hernia, or groin disruption, is a health issue of the pubic joint. It is a condition characterized by chronic groin pain in athletes and identified by a dilated ring of the inguinal canal. Soccer and ice hockey players are the athletes most commonly affected by athletic
Table of Contents
Athletic Pubalgia Symptoms
Symptoms of athletic pubalgia generally manifest as pain following physical activity, most frequently through hip extension, and twisting and turning movements. The painful symptoms usually radiate into the adductor muscle region and the testicles, although it is often difficult for the individual to pinpoint the exact location of the symptoms. Athletes with athletic pubalgia experience soreness and stiffness after physical activity.
Any exertion which increases intra-abdominal pressure, such as sneezing or coughing, as well as physical activity, can lead to pain. While pain in the stomach and pelvis can occur due to a variety of health issues, including injuries to the low back, or lumbar spine, the hip joint, the sacroiliac joint, and the abdomen, along with the genito-urinary system, diagnosis of athletic pubalgia demands skillful differentiation and evaluation.
Clinical Presentation of Athletic Pubalgia
The diagnosis of athletic pubalgia is based on the patient’s history, where healthcare professionals may also depend on the use of magnetic resonance imaging, or MRI. Symptoms can frequently be reproduced by certain movements, such as performing crunches or sit-ups. Pain associated with athletic pubalgia may also be elicited with the patient in a “frog posture,” in which the individual is supine with knees bent and heels together.
Many athletes experience concomitant fatigue or tearing of the adductor muscles or labral tears of the hip. If there is stiffness in the adductor muscles post-injury, painful symptoms can manifest. Alternative treatment options should be to restore normal movement after the adductor has begun to heal, normally 6 to 8 weeks post-injury. Moreover, sleeping in a prone position with the hip on the affected side flexed and externally rotated can offer relief to some athletes with athletic pubalgia.
The precise prevalence of this health issue is unknown. Conservative therapies, such as gentle stretching, may temporarily alleviate
Curated by Dr. Alex Jimenez

Additional Topics: Acute Back Pain
Back pain is one of the most prevalent causes of disability and missed days at work worldwide. Back pain attributes to the second most common reason for doctor office visits, outnumbered only by upper-respiratory infections. Approximately 80 percent of the population will experience back pain at least once throughout their life. The spine is a complex structure made up of bones, joints, ligaments, and muscles, among other soft tissues. Because of this, injuries and/or aggravated conditions, such as herniated discs, can eventually lead to symptoms of back pain. Sports injuries or automobile accident injuries are often the most frequent cause of back pain, however, sometimes the simplest of movements can have painful results. Fortunately, alternative treatment options, such as chiropractic care, can help ease back pain through the use of spinal adjustments and manual manipulations, ultimately improving pain relief.

EXTRA IMPORTANT TOPIC: Hip Pain Chiropractic Treatment
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card